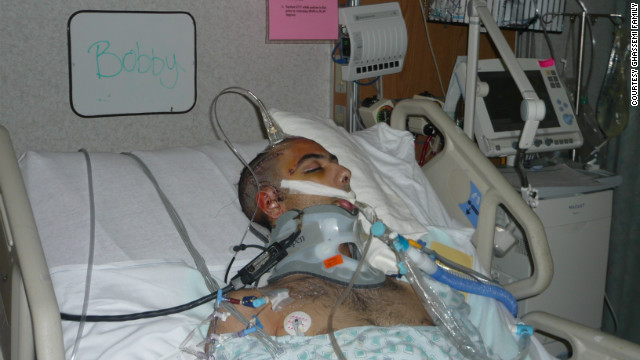
 Bobby Ghassemi was just 17 years old when he was in a horrific car accident.
Bobby Ghassemi was just 17 years old when he was in a horrific car accident.
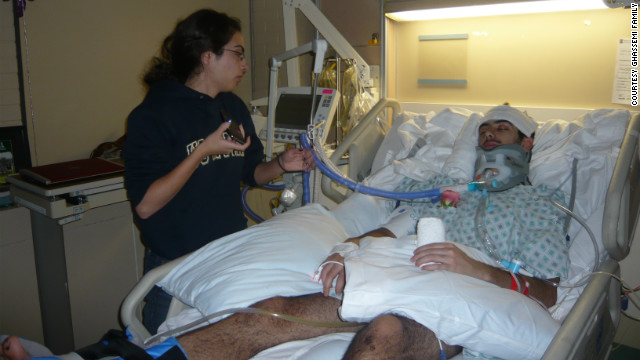 After the accident
in March 2010, doctors told Bobby's family that he could live out the
rest of his life in a vegetative state.
After the accident
in March 2010, doctors told Bobby's family that he could live out the
rest of his life in a vegetative state.
(CNN) -- Time seemed to slow as Marjan Ghassemi saw her 17-year-old son, Bobby, lying in a hospital bed after a car crash.
He had a thick band of
gauze wrapped around his head and a tangle of tubes protruding from his
body. A hole was cut into his windpipe, and the hollow-sounding hiss of
machines helping him breathe filled the room.
At that point, there was no telling whether he would live or die, but Marjan was determined not to cry.
"From day one, when we
got there, I didn't want him to know we were crying, that we were
upset," she said. "I wanted all positive energy in the room.
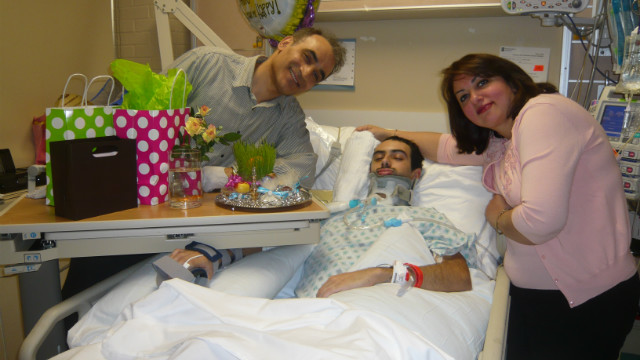 Ten days after the
accident, Bobby was still in a coma. Bobby's father, Peter, talked with
Dr. Michael Lewis, who suggested that omega-3 fatty acids might be able
to help. Peter insisted that his son be given high doses of fish oil
through a feeding tube.
Ten days after the
accident, Bobby was still in a coma. Bobby's father, Peter, talked with
Dr. Michael Lewis, who suggested that omega-3 fatty acids might be able
to help. Peter insisted that his son be given high doses of fish oil
through a feeding tube.
"I went in his ear and said ... 'You fight your way and come back to us.' "
It was March 2010. Bobby
Ghassemi had been driving fast along a winding road in Virginia when his
car barreled off the road. By the time paramedics arrived, he was in a
coma and barely alive.
"For all intents and
purposes, he was dead on the scene," said Dr. Michael Lewis, a physician
who later advised the family. "I'm looking at the reports, and they
report a Glasgow Coma Score of 3. A brick or a piece of wood has a
Glasgow Coma Score of 3. It's dead."
Ghassemi was airlifted to a hospital. For the first three days, it was touch and go.
Ghassemi's brain was so
engorged, doctors needed to relieve the pressure by taking out a portion
of his skull. He also had what is called diffuse axonal injury:
bleeding that suffused nearly every part of his brain.
"His doctor said to me,
'Listen, he has survived. It is a miracle that he lived, that he made
it,' " Marjan Ghassemi said. " 'If he comes out of the coma ... I don't
know if he's going to be a vegetable for the rest of his life or whether
he'll remember anybody.' "
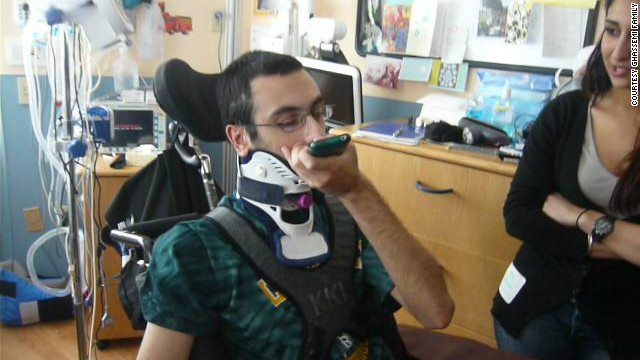 Bobby says the omega-3 fatty acids have helped in recovering his motor skills.
Bobby says the omega-3 fatty acids have helped in recovering his motor skills.
Ten days later, as Bobby
lay comatose but stable, his father, Peter Ghassemi, was sick of
waiting and desperate for an intervention. After a series of phone calls
to friends, he ended up speaking with Lewis, an Army colonel and
doctor.
After some discussion,
Lewis proposed something that Peter Ghassemi had never heard about for
traumatic brain injuries: fish oil.
At that point, Peter Ghassemi was open to anything.
"Every minute passing
was hurting my son ... because they weren't really doing anything to
help him besides keeping him alive and stabilizing all of his vital
signs," he said. "If there was a chance to improve, I wanted it to be
done right then."
'He was really in dire straits'
Fish oil -- which is
composed of omega-3 essential fatty acids, also found in the brain --
had been used only once before to treat a brain injury as devastating as
Ghassemi's. That was in 2006, in the case of Randal McCloy, the sole
survivor of a mine disaster in West Virginia.
McCloy, 26, was trapped
in a mine for 41 hours while the air around him and 12 other miners
filled with noxious methane and carbon monoxide. By the time he was
pulled from underground, he had had a heart attack, was in liver and
kidney failure and had a collapsed lung, according to his doctors.
His brain was also riddled with damage from the carbon monoxide and methane.
McCloy's prognosis was
not very different from Ghassemi's. According to his neurosurgeon at the
time, Dr. Julian Bailes, restoring McCloy's normal brain function was
truly a long shot.
"Randy was really on
death's doorstep," said Bailes, now co-director of NorthShore
Neurological Institute in Evanston, Illinois. "He was really in dire
straits."
Like with Ghassemi, once
McCloy was stabilized, there was little doctors could do to stem the
tide of inflammation and cell death occurring in his brain.
But Bailes and other
doctors on McCloy's team resisted the "wait and see" course common in
these types of cases and began an unorthodox treatment regimen,
including hyperbaric oxygen treatments and high doses of fish oil.
"The concept was then
trying to rebuild his brain with what it was made from when he was an
embryo in his mother's womb," Bailes said.
The brick wall analogy
That's the theory behind
using omega-3 fatty acids to heal brain injury. The human brain, which
itself is a fatty mass, is about 30% composed of omega-3 fatty acids,
according to Lewis.
In his words, high doses
of omega-3 fatty acids, since they mirror what is already in the brain,
could facilitate the brain's own natural healing process.
"It really gets down to
what I would call my brick wall analogy," Lewis said. "If you have a
brick wall and it gets damaged, wouldn't you want to use bricks to
repair the wall? And omega-3 fatty acids are literally the bricks of the
cell wall in the brain."
Most of the studies
about omega-3 for traumatic brain injury are in animals, but they
indicate potential for healing the human brain.
After a trauma, the
brain tends to swell, and the connections between some nerve cells can
become damaged, while other cells simply die.
National Institutes of Health research suggests that omega-3 fatty acids may inhibit cell death and could be instrumental for reconnecting damaged neurons.
Another recent
study
revealed genes that are activated to contain massive damage --
especially inflammation -- when the brain is injured. What activates
those genes: omega-3.
"We have strong data
that suggest omega-3 will activate good proteins to cope with brain
damage and turn off proteins that cause neuroinflammation," said Dr.
Nicolas Bazan, director of the Neuroscience Center of Excellence at LSU
Health in New Orleans and author of the study.
And besides that,
according to Bailes and Lewis, fish oil may be the only solution for
brain damage that continues after a traumatic brain injury patient has
been stabilized.
"There is no known
solution; there's no known drug; there's nothing that we have really to
offer these sorts of patients," said Bailes, who along with Lewis
received money from companies that make fish oil after their treatment
of Ghassemi and McCloy.
The damage to McCloy's
brain was profound, according to Bailes. Not only did it experience
massive cell death, the protective sheath around McCloy's nerve cells
had been stripped during the hours of exposure to toxic gases. That
sheath, called myelin, allows brain cells to communicate with one
another.
Bailes consulted with a
fish oil expert and eventually decided that administering 20 grams a day
of omega-3 fish oil through a feeding tube might repair the myelin
sheath. (For comparison: A typical supplemental dose for someone with an
uninjured brain is about 2 grams a day.)
"We decided to throw the
kitchen sink at him," Bailes said. "If we were going to fail, we were
going to fail with all guns blazing, so we gave him a very high,
unprecedented dose to make sure we saturated and got high levels in the
brain."
Less than three weeks
after the mine disaster, McCloy was emerging from his coma. Three months
after that, he was walking and speaking.
Citing McCloy's dramatic
recovery, Lewis spoke with Peter Ghassemi about introducing omega-3 for
his son. After that conversation, Peter Ghassemi was convinced and
began to pressure his son's doctors.
"It was a fight," Peter
Ghassemi said. "They didn't believe, and they said, 'Fine, the West
Virginia miner was one case. Bring me 999 more cases, a thousand more
cases ... before I can give it to your son.' "
But eventually they
conceded, and Bobby Ghassemi was started on high-dose fish oil therapy,
at a dosage that mirrored what Bailes had given to McCloy in 2006.
'The whole place was cheering for me'
Two weeks after beginning the regimen, Ghassemi was emerging from his coma.
"We saw hand movements
on the left side," Peter Ghassemi said. "Around the fifth or sixth week,
there was some movement, and then his hands started moving more, the
leg was moving more."
Soon after that, Bobby
began to show signs of recognizing his family and his dog and of
discerning things like colors and numbers. Slowly, his brain was
recovering, and his family ardently believes that the high-dose fish oil
is the reason why.
"His brain was still
recovering, but with (omega-3), it recovered much faster and in a
shorter amount of time," Peter Ghassemi said. "His brain was damaged,
and this was food for the brain."
Three months after his accident, Bobby Ghassemi was well enough to attend his high school graduation.
"The whole place was
cheering for me, and they all stood up and were screaming and cheering
my name," Ghassemi, now 20, recalls with a smile. "I took my graduation
cap off and waved it around."
He still has significant
left-side weakness and is relearning how to walk, but his progress has
been tremendous, according to Lewis.
"In my opinion, and this
is pure speculation, he never would have come out of a coma if it
hadn't been for the use of omega-3s to allow that natural healing
process to occur," said Lewis, founder of the Brain Health Education and Research Institute. "In the end, the brain has to heal itself. There are no magic cures for brain injury."
Large-scale study needed
But what do these two
dramatic stories really say about omega-3 as a potential treatment for
traumatic brain injury? For now, they are merely stories with omega-3 as
a common denominator.
The remaining questions
are as poignant as the stories themselves: Could youth have been a
factor for Ghassemi and McCloy? What about other treatments given to
McCloy, like hyperbaric oxygen? Could they have played a role?
Those and other questions could and should be answered, according to experts, with a large-scale clinical study.
"These two clinical
cases where we have a wildly unexpected recovery, was it just luck that
they woke up?" asked Dr. Joseph Hibbeln, an omega-3 expert and chief of
the Section on Nutritional Neurosciences at the National Institutes of
Alcohol Abuse and Alcoholism. "Or is there some reasonable scientific
explanation for it?
"Given that there aren't
any other treatments, this is a good bet," Hibbeln said. "It's really
only reasonable to go forward with doing the full press of careful
intervention studies."
The implications of a
successful study are huge: 1.7 million people suffer a traumatic brain
injury each year in the United States.
And research into how omega-3 might function for stroke, Parkinson's disease and early Alzheimer's disease is ongoing.
"The message that I'm
trying to get across is, there's more you can do," Lewis said. "If you
add omega-3s, we can then begin to let the brain heal itself a little
more efficiently."
"Up until the time the
pharmaceutical industry gives us a drug that cures all brain injury,
this is the best hope we have," Bailes said.
 Time Magazine‘s Maia Szalavitz does good work Monday with a piece reviewing some clinical evidence on cannabinoids – the molecules in marijuana – and aging.
The brain’s own cannabinoid system is responsible for stopping
inflammation, and “a sort of anti-oxidant cleanse, removing damaged
cells and improving the efficiency of the mitochrondria, the energy
source that powers cells, ultimately leading to a more robustly
functioning brain.” Stimulating it with cannabinoids increase
brain-derived neurotrophic factor which protects brain cells and
promotes neuron growth, and – bucking the stereotype – maintains normal
cognitive function in old age.
Time Magazine‘s Maia Szalavitz does good work Monday with a piece reviewing some clinical evidence on cannabinoids – the molecules in marijuana – and aging.
The brain’s own cannabinoid system is responsible for stopping
inflammation, and “a sort of anti-oxidant cleanse, removing damaged
cells and improving the efficiency of the mitochrondria, the energy
source that powers cells, ultimately leading to a more robustly
functioning brain.” Stimulating it with cannabinoids increase
brain-derived neurotrophic factor which protects brain cells and
promotes neuron growth, and – bucking the stereotype – maintains normal
cognitive function in old age.
 Bobby Ghassemi was just 17 years old when he was in a horrific car accident.
Bobby Ghassemi was just 17 years old when he was in a horrific car accident.  After the accident
in March 2010, doctors told Bobby's family that he could live out the
rest of his life in a vegetative state.
After the accident
in March 2010, doctors told Bobby's family that he could live out the
rest of his life in a vegetative state.  Ten days after the
accident, Bobby was still in a coma. Bobby's father, Peter, talked with
Dr. Michael Lewis, who suggested that omega-3 fatty acids might be able
to help. Peter insisted that his son be given high doses of fish oil
through a feeding tube.
Ten days after the
accident, Bobby was still in a coma. Bobby's father, Peter, talked with
Dr. Michael Lewis, who suggested that omega-3 fatty acids might be able
to help. Peter insisted that his son be given high doses of fish oil
through a feeding tube.  Bobby says the omega-3 fatty acids have helped in recovering his motor skills.
Bobby says the omega-3 fatty acids have helped in recovering his motor skills. 
 .
According to a 2010 study in CA: A Cancer Journal for Clinicians, the
average survival rate after a glioblastoma diagnosis is 14 months
(though improving surgical techniques had boosted that number from 10
months in only five years prior to the study).
.
According to a 2010 study in CA: A Cancer Journal for Clinicians, the
average survival rate after a glioblastoma diagnosis is 14 months
(though improving surgical techniques had boosted that number from 10
months in only five years prior to the study).


 The Human Brain
The Human Brain
 Portraits of the Mind
Portraits of the Mind
 Canine Scents
Canine Scents
 Dripping Dendrites
Dripping Dendrites
 Baroque Blood Vessels
Baroque Blood Vessels
 View of a StrokeCredit
View of a StrokeCredit
 Mouse BrainCredit
Mouse BrainCredit
 Spiny NeuronCredit
Spiny NeuronCredit
 Artsy Brain CellsCredit
Artsy Brain CellsCredit
 Color My Cerebellum
The colored splotches reveal so-called presynaptic terminals, or junctions through which neuron signals are sent, formed by the cerebellum's axons.
Color My Cerebellum
The colored splotches reveal so-called presynaptic terminals, or junctions through which neuron signals are sent, formed by the cerebellum's axons. BrainbowCredit
BrainbowCredit


 Neurotopia recently began beta-testing a dry sensor, mobile headphone and tablet system that would map brain waves
Neurotopia recently began beta-testing a dry sensor, mobile headphone and tablet system that would map brain waves
