We routinely write about the ubiquitous plastic hardener bisphenol A (BPA) and its myriad links to adverse health effects. Used in polycarbonate manufacturing, BPA is commonly found in the lining of food and beverage cans, thermal paper receipts, a wide array of plastic products, and resins used in nautical paint. And, while it has long been recognized that BPA affects animal hormone levels, emerging science points to the same issues in humans, wrote Environmental Health News.
Of note, BPA in nautical paint means the chemical could be linked to high BPA levels found in “beach sand and coastal seawater” worldwide, said USNews previously.
Hundreds and hundreds of studies have linked the ubiquitous chemical to a growing number of diseases and disorders and continue to confirm that BPA appears to cause significant disruption to the body’s endocrine system.
BPA has been linked to cardiovascular disease, intestinal problems, brain cell connection interference, increased risks of reproductive and immune system diseases and disorders, problems with liver function testing, interruptions in chemotherapy treatment, links with serious health problems, and erectile dysfunction and other sexual problems in males. In urine tests, BPA is found in the overwhelming majority of Americans, more than 93 percent and, significantly, the chemical is found in 90 percent of all newborns.
According to Environmental Health News, BPA was first produced in 1891 and has long been linked to its “estrogenic properties in animals.”
For this most recent study, researchers measured BPA concentrations in the urine of 167 men from a Massachusetts infertility clinic, as well as hormone levels in the men’s blood, said Environmental Health News. The research revealed that men with higher urine BPA concentrations also tested with increased blood levels of follicle-stimulating hormone (FSH) and decreased levels of inhibin B; these particular measures are linked with poorer human sperm quality, added Environmental Health News.
The study also found a decrease in the estrogen-to-testosterone ratio, which could point to issues in how these hormones are produced or removed from the body, said Environmental Health News, adding that the research also found a decrease in thyroid-stimulating hormone (TSH), which suggests excessive thyroid hormone production, or a hyperthyroidic effect. These study results support prior animal studies pointing to links between hormone levels and BPA exposure.
Industry has long argued that scientists and advocates exaggerate BPA’s adverse effects, continually citing two industry studies; however, at last count, over 900 peer-reviewed studies found links between BPA and such effects.
Regardless, a number of countries, states, and other entities have issued bans on BPA, which imitates the hormone estrogen and acts as an anti-androgen. This means, even in the smallest of amounts, BPA affects sexual development and processes, especially in the bodies of developing fetuses, infants, and children, explained Science Daily previously. Canada was the first country to issue a BPA ban; Denmark recently followed; three U.S. states have issued bans; and France is considering a ban, as is Massachusetts.
Wednesday, May 5, 2010
Neuroscience: Illuminating the brain
Systems neuroscientists are pushing aside their electrophysiology rigs to make room for the tools of 'optogenetics'. Lizzie Buchen reports from a field in the process of reinvention.
Lizzie Buchen

Sabes's training was in physics, machine learning and human perception, and his lab has been working with humans and non-human primates to develop models of how the brain turns perceptions into actions; for example, seeing a fly and swatting it away. He's not alone in his molecular-biology naivety at the Keck Center — there is no cell-culture facility, no PCR machine and no bench-top centrifuge. The centre's one ice machine spits out large cubes instead of the crushed ice routinely used for chilling reagents — it was ordered by mistake, and no one has cared enough to fix the situation. Sabes and his colleagues have had no need for such apparatus. Researchers in their field of 'systems neuroscience' try to understand how networks of neurons process sensations and control behaviours such as learning and decision-making. And up to this point, much of their progress has been made using electrophysiology, stimulating and recording from the brains of animals as they perform a task or develop a new skill.
Now though, advances in a five-year-old field called optogenetics are convincing these scientists to crack open molecular-biology textbooks. Using a hybrid of genetics, virology and optics, the techniques involved enable researchers to instantaneously activate or silence specific groups of neurons within circuits with a precision that electrophysiology and other standard methods do not allow. Systems neuroscientists have longed for such an advance, which allows them their first real opportunity to pick apart the labyrinthine jumble of cell types in a circuit and test what each one does. "It has revolutionized my approach to science," says Antonello Bonci, a neurophysiologist at the UCSF Ernest Gallo Clinic and Research Center in Emeryville who began using the technique in 2007. "It can clarify unequivocally the role of specific classes of cells, and solve controversies that have been going on for many, many years." Among the clarifications sought is the precise function of 'place' cells, hippocampal neurons that fire only when an animal finds itself in a specific location; another is the function of complex activity patterns observed when an animal is paying attention or executing a movement.
“Optogentics can solve controversies that have been going on for many, many years.”
A field's evolution
The transition phase isn't easy. Optogenetic tools were first used in cell cultures and mice, which are amenable to genetic manipulation. Now systems neuroscientists must adapt them to function in organisms they traditionally study such as rats, birds and primates. With the technical challenge comes a personal one, as researchers leave their experimental comfort zone for a new field.Most, however, anticipate that any discomfort will be worthwhile. "This is God's gift to neurophysiologists," says Robert Desimone, director of the McGovern Institute for Brain Research at the Massachusetts Institute of Technology (MIT) in Cambridge, who has been using electrophysiology for more than 30 years. "Molecular techniques were always beyond us, so this is our first opportunity. It's a revolution. But we're catching up to the revolution that had been going on for the rest of the world."
Optogenetics started out in 2005, when a team at Stanford University in California led by Karl Deisseroth and his then-postdoc Ed Boyden inserted a light-sensitive channel from green algae, called channelrhodopsin-2 (ChR2), into neurons growing in a dish. Exposed to a pulse of blue light, the channels opened and a flood of positive ions poured into the neurons, making them fire1. Within a year, 30 labs had contacted Deisseroth to ask for the technology. By March 2010, Deisseroth had sent protocols or genetic constructs to more than 500 labs around the world, and Boyden, now at MIT, had sent them to in excess of 250.
Click for a larger version.
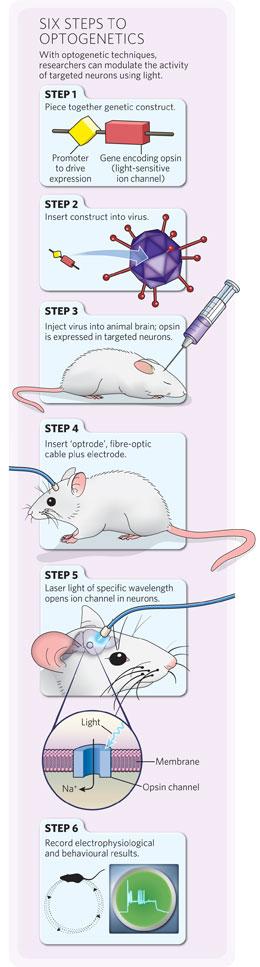
The technique has been refined greatly in the past five years, but the basic steps are the same (see 'Six steps to optogenetics'). First, researchers create a genetic construct containing the ChR2 gene or another 'opsin' gene, along with genetic elements that control its expression — for example, a specific 'promoter' sequence. Then, they package up the construct in a virus. When the virus is injected into an animal's brain, it widely infects neurons and delivers the construct, but the opsin is expressed in only a subgroup of cells with the necessary machinery to activate its promoter. The opsin proteins sit in the membrane of those neurons, and researchers trigger them with light of a specific wavelength, typically delivered through an optic fibre threaded through an animal's skull. Deisseroth and Boyden have discovered or engineered many other opsins that allow neurons to be manipulated in different ways, including neural silencers.The technique is popular, but complex. The fastest adopters were those who work with cells grown in vitro and animals such as flies, worms and mice, for which they could take advantage of established genetic tools and well-characterized animal lines. "The number of tangible results are still of the order of half a dozen or so. But we're on the rising phase of the exponential," says Karel Svoboda, a neuroscientist at the Howard Hughes Medical Institute's Janelia Farm research campus in Ashburn, Virginia, who last year started mapping mouse cortical circuits using optogenetics.
From the start, these developments sent quivers through the systems-neuroscience community. "When I first saw this stuff, at a meeting where Karl was presenting some of the earliest results, I thought, 'Oh God, finally'," says Loren Frank, another neuroscientist at the Keck Center. "And then I thought, oh great. Here I was, I'd gotten pretty good at the stuff I thought I needed to do, and now I have to learn an entirely new field."
 Frank — who says he has "always had a bit of molecular-biology envy" — began collaborating with Deisseroth to use optogenetics on rats just over three years ago, for his studies of place cells and hippocampal circuits. Silencing or activating specific cells could help show whether or how they help an animal explore a new location or recognize a familiar one. "If you want to actually understand the system, you have to start trying to get control of the system and actually dissect the circuit," says Frank. Standard techniques have not allowed that type of dissection. Electrodes inserted into an animal's brain typically stimulate hundreds of thousands of cells; using lesions or drugs also hits circuits like a hammer. Optogenetics could be a scalpel, turning particular neurons in a circuit on or off within milliseconds.
Frank — who says he has "always had a bit of molecular-biology envy" — began collaborating with Deisseroth to use optogenetics on rats just over three years ago, for his studies of place cells and hippocampal circuits. Silencing or activating specific cells could help show whether or how they help an animal explore a new location or recognize a familiar one. "If you want to actually understand the system, you have to start trying to get control of the system and actually dissect the circuit," says Frank. Standard techniques have not allowed that type of dissection. Electrodes inserted into an animal's brain typically stimulate hundreds of thousands of cells; using lesions or drugs also hits circuits like a hammer. Optogenetics could be a scalpel, turning particular neurons in a circuit on or off within milliseconds. From brain to behaviour
By April 2009, Frank was making progress in rats, achieving ChR2 expression in a discrete set of hippocampal neurons and getting them to fire. And down the hall, Sabes was ready to try the technique in primates as part of his efforts to understand circuits involved in hand-eye coordination. "I knew optogenetics was on the horizon, and it was potentially exciting, but realistically, I just didn't know anything about this stuff," he says.Sabes and two songbird researchers at the Keck Center, Michael Brainard and Allison Doupe, teamed up with Frank, Deisseroth and another colleague, Linda Wilbrecht, a neuroscientist at the Gallo Center. The group, one of the first big collaborations aiming to apply optogenetics to rats, birds and primates, received a US$1.6-million National Institutes of Health grant in September 2009 through the financial stimulus. The neuroscientists describe what they'd like to do — in Sabes's case, for example, alter patterns of activity that occur in the parietal lobe when an animal reaches for something, and work out which patterns are important for planning, initiating or adjusting the movement. Wilbrecht's lab leads efforts to generate the appropriate constructs and select the best viruses, and Deisseroth tries to build new viral and optogenetic tools that they need.
One huge advantage for mouse researchers has been the ready-made bank of animal lines engineered to express an enzyme called Cre recombinase in subsets of neurons, such as all dopaminergic ones, which they can use in combination with specially designed genetic constructs to achieve the cellular specificity they want. In other animals, a promoter must be found that will only be turned on in dopaminergic neurons. Some promoters and viruses that work in mice do not work in rats or primates, meaning that researchers have to start from scratch. Progress has been faster in rats because the animals are relatively easy to breed and are similar enough to mice for methods to be transferable. In March 2009, Deisseroth was the first to publish a rat optogenetic study, in which he manipulated circuit components in a rat model of Parkinson's disease to work out which parts might account for the relief afforded by deep-brain stimulation3.
An additional complication for primate researchers is that primate brains are larger than those of rodents, making it difficult to ensure the injected virus and the activating light penetrate deep enough. And troubleshooting in monkeys will take much longer than in rats, given the long lifetime and high value — experimental, financial and ethical — of the animals. But in April 2009, Desimone and his colleagues worked with Boyden to publish the first experiment showing that viruses can be used to insert opsin channels and control neural activity in a macaque.
“It felt like garage-development days, cutting stuff up to see what works.”
In January, with the optrode inserted into the region where the virus had been injected two months earlier, Sabes flipped on a blue laser and watched a screen showing electrical readout from the optrode. Yellow waveforms flashed across the screen, paired with a flurry of clicking noises: spikes of neural activity.
Experts on hand
Like Sabes, the few other electrophysiologists starting to tackle primate optogenetics are keeping experts in the technique close by to avoid making a novice's mistakes (see 'Opto school'). "It's critical that at least the initial phase is collaborative," says Krishna Shenoy, a primate electrophysiologist at Stanford University who has been working closely with Deisseroth for two years to explore how neurons in the brain's motor cortex control arm movements.
Boyden's paper is still the only optogenetics publication on primates, and the technique is some way from generating new discoveries. It's still not known whether the opsins will be expressed consistently for the year or two required to train monkeys in sophisticated behaviours and then record from neurons repeatedly. "If it only expresses at the right level for a few months and then dies off or expresses too much, it's just untenable," says Shenoy.All these questions take time and money to answer, and not every lab has an appetite for the work. "It's probably going to have a big impact, and I'm definitely interested," says Tirin Moore, a neurobiologist at Stanford. "But I'm less interested in pioneering the approach in monkeys and more interested in using the tools once it's clear that they work."
Meanwhile, Boyden and Deisseroth are hammering out some of the problems. Last month, Deisseroth reported a system in mice that could make detailed knowledge of promoters unnecessary: two viruses containing separate genetic constructs are injected into two connected brain regions. Only neurons that run between the two regions will receive doses of both constructs, which then interact to express the opsin5. Boyden is designing a light source that would weigh a fraction of a gram so that animals can walk around freely rather than being tethered to a fibre-optic cable.
"Soon enough, this is going to be standard technology," says Sabes. "The hardware will be there, the viruses will be there, there will be a handful of constructs that everyone agrees works reasonably well." That aim is likely to be furthered by a two-year, $14.9-million grant from the US Defense Advanced Research Projects Agency in Arlington, Virginia, that Sabes, Deisseroth and six other labs, led by Shenoy, won in April. The team will attempt to use primate optogenetics to explore brain repair after injury, including possible light-based neural prosthetics, devices that might stimulate appropriate patterns of activity in the surviving neurons.
For now, Sabes is still trying to analyse the results of his first monkey experiment. He has sent the animal's brain to a friend competent in histology, who will slice it, paper thin, onto slides. Then Sabes will have to grapple with a fluorescent microscope for the first time, trying to work out where and how well the opsin was actually expressed.
"I'm sure it's not that hard," says Sabes, "but I've never done it".
Lizzie Buchen is a freelance writer based in San Francisco.
MS patients to rally for experimental treatment
People with multiple sclerosis will rally across Canada on Wednesday to demand access to a controversial procedure not currently available in Canada or covered by provincial health insurance policies.
The procedure, developed by Italian researcher Dr. Paolo Zamboni, involves angioplasty to help ease the flow in neck veins of blood from the brain to the heart. Zamboni believes narrowed or blocked veins force blood to move backwards or reflux back into the brain and spine, causing damage.
He's termed the condition chronic cerebrospinal venous insufficiency, or CCSVI.
The rallies are scheduled to take place in Halifax, Ottawa, Toronto, Regina, Edmonton, Vancouver, Victoria and elsewhere.
"The point of the rally is to demonstrate and voice our opinions about the way the government is handling the CCSVI situation," Andrew Katz, who has MS and uses a wheelchair, told CBC News in April. "It's not moving fast enough."
Many MS specialists say Zamboni's procedure is experimental at best and could be dangerous.
Studies are underway to show how common CCSVI is in MS patients, those with other neurological conditions and healthy people, as well as to explore its potential role as a major risk factor in MS.
But despite specialists' hesitation, some Canadian patients are travelling overseas, paying for tests and surgery out of their own pocket. Others are lobbying for the Canadian health-care system to cover the diagnostic tests to look for blocked veins in people with MS.
More than 20 Canadians traveled to a clinic in Poland between February and April for the treatment.
The representatives are hoping to secure commitments from the MPs on two major issues:
Robert Zivadinov said a combination of being born with narrow veins in the neck or thorax, along with environmental and genetic factors such as vitamin D deficiency or exposure to the Epstein Barr virus may play a role in causing MS, an autoimmune disorder.
The procedure, developed by Italian researcher Dr. Paolo Zamboni, involves angioplasty to help ease the flow in neck veins of blood from the brain to the heart. Zamboni believes narrowed or blocked veins force blood to move backwards or reflux back into the brain and spine, causing damage.
He's termed the condition chronic cerebrospinal venous insufficiency, or CCSVI.
The rallies are scheduled to take place in Halifax, Ottawa, Toronto, Regina, Edmonton, Vancouver, Victoria and elsewhere.
"The point of the rally is to demonstrate and voice our opinions about the way the government is handling the CCSVI situation," Andrew Katz, who has MS and uses a wheelchair, told CBC News in April. "It's not moving fast enough."
Many MS specialists say Zamboni's procedure is experimental at best and could be dangerous.
Studies are underway to show how common CCSVI is in MS patients, those with other neurological conditions and healthy people, as well as to explore its potential role as a major risk factor in MS.
But despite specialists' hesitation, some Canadian patients are travelling overseas, paying for tests and surgery out of their own pocket. Others are lobbying for the Canadian health-care system to cover the diagnostic tests to look for blocked veins in people with MS.
More than 20 Canadians traveled to a clinic in Poland between February and April for the treatment.
Meetings with MPs
The rallies also coincide with meetings between representatives of the MS Society of Canada and approximately 40 members of Parliament.The representatives are hoping to secure commitments from the MPs on two major issues:
- Creating a nationwide income security program for people affected by MS that would replace what the society calls "the current hodgepodge of disability pensions, social assistance programs and tax credits, some of which cannibalize each other resulting in less money for people with disabilities.
- Increasing funding for health research with a focus on "innovative health research that can be translated rapidly into therapies that can benefit people with MS and other chronic conditions," including researching into CCSVI.
Robert Zivadinov said a combination of being born with narrow veins in the neck or thorax, along with environmental and genetic factors such as vitamin D deficiency or exposure to the Epstein Barr virus may play a role in causing MS, an autoimmune disorder.
Stem cells raise hope for treatment for multiple sclerosis patients
Thousands of MS sufferers could benefit from a revolutionary treatment that injects them with stem cells taken from their own bone marrow.
Researchers have long believed that the stem cells could halt and even reverse the effects of the disease by patching up the damaged parts of the brain and spinal cord.
Now British scientists carrying out one of the first ever trials into the procedure believe that they have proved that it works.
The research team, led by Professor Neil Scolding, at the University of Bristol and North Bristol NHS Trust, believe that the treatment has stabilised the condition and shown some "benefits".
"We are encouraged by the results of this early study," he said.
"We believe that stem cells mobilised from the marrow to the blood are responsible, and that they help improve disease in several ways."
MS or multiple sclerosis is an incurable disease that affects around 85,000 people in Britain slowly attacking the central nervous system and leaving many sufferers eventually wheelchair bound.
For some reason the immune system turns on healthy nerve cells and damages them.
Previous studies in the laboratory have shown that stem cells are able to develop into other cell types, travel through the bloodstream to the brain and are actively taken up by damaged areas.
The trial, which lasted a year, is one of the first to use patients' own bone marrow stem cells to treat their MS.
It involved six people with MS, aged between 30 and 60, having a pint of bone marrow extracted from their pelvises.
The material is filtered of bone and fat leaving pure stem cells which are then injected on the same day back into the patients' arms.
Over the year, the patients were monitored closely and given regular brain scans to see what impact the treatment has had on them.
The study, journal Clinical Pharmacology and Therapeutics, carried out at Frenchay Hospital avoids the ethical controversy that surrounds many stem cell studies because it does not use human embryos.
Researchers found that the patients suffered "no serious adverse effects" from the treatment and tests suggested the disease was stable and there had been improvement in the effectiveness of damaged nerve cells.
They showed that the damaged nerve pathways were able to carry electrical pulses more effectively after the treatment.
Now the researchers want to carry out a longer and larger study to see if the treatment can be improved and works consistently.
Professor Neil Scolding said: “The safety data are reassuring and the suggestion of benefit tantalising."
Dr Claire Rice, co-author, said: "The results are very encouraging. We would have expected these pathways to get worse but they have actually got better.
"It is exciting because the treatment is relatively pain free and patients do not need to stay overnight in hospital."
Bone marrow is known to contain stem cells capable of replacing cells in many types of tissues and organs – and so is of great interest to those working to develop new treatments for many diseases, including those affecting the nervous system.
An earlier study on 21 adults in the Lancet also showed that stem cells could halt the progress of the disease and even show some improvement.
The idea is that if caught early enough the stem cells could protect patients from the permanent damage caused to nerve cells and prevent disability.
Researchers have long believed that the stem cells could halt and even reverse the effects of the disease by patching up the damaged parts of the brain and spinal cord.
Now British scientists carrying out one of the first ever trials into the procedure believe that they have proved that it works.
The research team, led by Professor Neil Scolding, at the University of Bristol and North Bristol NHS Trust, believe that the treatment has stabilised the condition and shown some "benefits".
"We are encouraged by the results of this early study," he said.
"We believe that stem cells mobilised from the marrow to the blood are responsible, and that they help improve disease in several ways."
MS or multiple sclerosis is an incurable disease that affects around 85,000 people in Britain slowly attacking the central nervous system and leaving many sufferers eventually wheelchair bound.
For some reason the immune system turns on healthy nerve cells and damages them.
Previous studies in the laboratory have shown that stem cells are able to develop into other cell types, travel through the bloodstream to the brain and are actively taken up by damaged areas.
The trial, which lasted a year, is one of the first to use patients' own bone marrow stem cells to treat their MS.
It involved six people with MS, aged between 30 and 60, having a pint of bone marrow extracted from their pelvises.
The material is filtered of bone and fat leaving pure stem cells which are then injected on the same day back into the patients' arms.
Over the year, the patients were monitored closely and given regular brain scans to see what impact the treatment has had on them.
The study, journal Clinical Pharmacology and Therapeutics, carried out at Frenchay Hospital avoids the ethical controversy that surrounds many stem cell studies because it does not use human embryos.
Researchers found that the patients suffered "no serious adverse effects" from the treatment and tests suggested the disease was stable and there had been improvement in the effectiveness of damaged nerve cells.
They showed that the damaged nerve pathways were able to carry electrical pulses more effectively after the treatment.
Now the researchers want to carry out a longer and larger study to see if the treatment can be improved and works consistently.
Professor Neil Scolding said: “The safety data are reassuring and the suggestion of benefit tantalising."
Dr Claire Rice, co-author, said: "The results are very encouraging. We would have expected these pathways to get worse but they have actually got better.
"It is exciting because the treatment is relatively pain free and patients do not need to stay overnight in hospital."
Bone marrow is known to contain stem cells capable of replacing cells in many types of tissues and organs – and so is of great interest to those working to develop new treatments for many diseases, including those affecting the nervous system.
An earlier study on 21 adults in the Lancet also showed that stem cells could halt the progress of the disease and even show some improvement.
The idea is that if caught early enough the stem cells could protect patients from the permanent damage caused to nerve cells and prevent disability.
Thinking about it
If you are amazed at the number of memory tracts that your computer holds, let me enlighten you on the number of memory tracts that are in the human brain. In his book, “Soul Healing,” Dr. Bruce Goldberg relates, “Everything that we can detect through our five senses… is permanently stored in the subconscious mind’s memory bank and functions at least 16 hours per day. One million pieces of information are stored each day. Scientists estimate that the average human mind contains 70 trillion memory tracts.”
For your brain to function optimally, it needs oxygen, which is supplied by a healthy heart and lungs which receive oxygen supply by participating in some form of exercise at least a half hour daily each week. Water is also necessary to prevent dehydration, which is supplied by drinking at least four glasses of water daily. The brain also needs essential nutrients in the form of omega 3 fatty acids found in dark, leafy greens, cold water fish such as salmon, sardines, mackerel and tuna.
To keep the brain healthy, it needs a good source of amino acids, which are found in poultry, egg whites, lean meats, grains and legumes. To prevent damage and to repair the brain cells, a host of vitamins and minerals are required which can to found in organic plant foods. The brain also needs an adequate amount of glucose, derived from complex forms found in fresh fruit, whole grains and vegetables.
To illustrate the need for proper nutrition as we all age, I would like you to enjoy the following story:
Two elderly folks were sitting in their living room enjoying television. The gentleman rose from his seat and told his wife that he was going into the kitchen to get some ice cream and would she like to have some? She replied, “That would be nice.” As he got to the kitchen door, he asked his wife whether she would like some chocolate syrup on the ice cream. Again, she gave a positive reply. She then told him that he should write her request down due to his forgetfulness. After several minutes, he returned with a plate of scrambled eggs. She looked at him and said, “I told you that you should have written it down. You forget the bacon.”
Speaking of forgetfulness, I would like to close with a wonderful poem written by my wonderful patient, Oliver Manning, who always maintained his memory right to the end. He is no longer with us:
All Mixed Up
Just a line to say I’m living
That I’m not among the dead
Tho, I’m getting more forgetful
And more mixed up in my head.
For, sometimes I can’t remember
When I stand at the foot of the stairs
If I must go up for something
Or, I’ve just come down from there.
And before the fridge, so often
My mind is filled with doubt
Have I just put food away or,
Have I come to take some out?
And there are time when it is dark out
With my nightcap on my head
I don’t know if I’m retiring
Or just getting out of bed..
So, if it’s my turn to write you
There is no need of getting sore
I may think that I have written
And don’t want to be a bore.
So remember, I do love you
And I wish that you were here
But now, it’s nearly mail time,
So, I must say “goodbye my dear.”
There I stood beside the mailbox
With a face so very red
Instead of mailing you my letter
I opened it instead.
It also appears that laughter reduces stress and also improves the memory. So I suggest that you laugh often, even if there is nothing to laugh about.
In closing, keep in mind the United Negro College Fund slogan: “A mind is a terrible thing to waste.”
For your brain to function optimally, it needs oxygen, which is supplied by a healthy heart and lungs which receive oxygen supply by participating in some form of exercise at least a half hour daily each week. Water is also necessary to prevent dehydration, which is supplied by drinking at least four glasses of water daily. The brain also needs essential nutrients in the form of omega 3 fatty acids found in dark, leafy greens, cold water fish such as salmon, sardines, mackerel and tuna.
To keep the brain healthy, it needs a good source of amino acids, which are found in poultry, egg whites, lean meats, grains and legumes. To prevent damage and to repair the brain cells, a host of vitamins and minerals are required which can to found in organic plant foods. The brain also needs an adequate amount of glucose, derived from complex forms found in fresh fruit, whole grains and vegetables.
To illustrate the need for proper nutrition as we all age, I would like you to enjoy the following story:
Two elderly folks were sitting in their living room enjoying television. The gentleman rose from his seat and told his wife that he was going into the kitchen to get some ice cream and would she like to have some? She replied, “That would be nice.” As he got to the kitchen door, he asked his wife whether she would like some chocolate syrup on the ice cream. Again, she gave a positive reply. She then told him that he should write her request down due to his forgetfulness. After several minutes, he returned with a plate of scrambled eggs. She looked at him and said, “I told you that you should have written it down. You forget the bacon.”
Speaking of forgetfulness, I would like to close with a wonderful poem written by my wonderful patient, Oliver Manning, who always maintained his memory right to the end. He is no longer with us:
All Mixed Up
Just a line to say I’m living
That I’m not among the dead
Tho, I’m getting more forgetful
And more mixed up in my head.
For, sometimes I can’t remember
When I stand at the foot of the stairs
If I must go up for something
Or, I’ve just come down from there.
And before the fridge, so often
My mind is filled with doubt
Have I just put food away or,
Have I come to take some out?
And there are time when it is dark out
With my nightcap on my head
I don’t know if I’m retiring
Or just getting out of bed..
So, if it’s my turn to write you
There is no need of getting sore
I may think that I have written
And don’t want to be a bore.
So remember, I do love you
And I wish that you were here
But now, it’s nearly mail time,
So, I must say “goodbye my dear.”
There I stood beside the mailbox
With a face so very red
Instead of mailing you my letter
I opened it instead.
It also appears that laughter reduces stress and also improves the memory. So I suggest that you laugh often, even if there is nothing to laugh about.
In closing, keep in mind the United Negro College Fund slogan: “A mind is a terrible thing to waste.”
Surgery for Treatable Dementia Might Also Help in Alzheimer’s
Some people with Alzheimer’s disease may be helped by a brain shunt normally used to treat another, less common neurological condition, new research suggests.
The other condition, normal pressure hydrocephalus (NPH), occurs when excess cerebrospinal fluid builds up in the ventricles, or cavities, deep within the brain. The reasons for the build-up of fluid are unknown, but it tends to occur in older people, said study author Dr. Sebastian Koga, a senior resident and surgeon in the department of neurosurgery at University of Virginia Health Science Center.
When diagnosing NPH, doctors look for three specific symptoms: difficulty walking (gait disturbances), urinary incontinence and dementia, or memory loss. The condition can often be slowed or relieved through a surgical procedure in which a shunt is implanted in the brain to drain fluid into the abdominal cavity, where it’s harmlessly reabsorbed, Koga said.
In the study, Koga and his colleagues took brain biopsies from 50 patients who had been diagnosed with NPH and who had shunt surgery.
About 30 percent had also been diagnosed with other conditions, including Parkinson’s-like tremors (13 percent), major depression (16 percent) and Alzheimer’s (3 percent).
After the surgery, the researchers followed patients for an average of 26 months. Nearly half (47 percent) had a significant improvement in their symptoms.
But about 21 percent saw no benefit and 30 percent continued to decline rapidly, Koga said.
In analyzing the brain tissue, the researchers found that the patients most likely to not improve or to decline also had high counts of amyloid plaques and neurofibrillary tangles, the hallmarks of Alzheimer’s disease.
While one possible conclusion is that these patients also had Alzheimer’s, another possibility is that both conditions share underlying similarities, and that shunting could also help some of those with Alzheimer’s, Koga said.
“Since 1965, we have been thinking this triage of symptoms — gait abnormality, urinary incontinence and memory problems — as a special disease and we have named it normal pressure hydrocephaly,” Koga said. “My hypothesis is that NPH is not a specific disease process, but part of a spectrum of dementia.”
The research was to be presented Tuesday at the American Association of Neurological Surgeons meeting in Philadelphia.
Since the 1960s, doctors have considered NPH a separate disease from Alzheimer’s, which occurs when beta-amyloid protein builds up and forms amyloid plaques and neurofibrillary tangles. The process is thought to kill neurons and lead to the degenerative symptoms of Alzheimer’s.
Instead of focusing on the symptoms of NPH, Koga argues, the two conditions may both be caused by tau-protein abnormalities. That means that some of those 5 million to 6 million people with Alzheimer’s may also benefit from shunting, something not typically offered to patients diagnosed with Alzheimer’s, he added.
“It’s theoretically possible that this same surgery could help forestall the symptoms or improve the symptoms of Alzheimer’s,” Koga said.
One challenge, however, is determining which Alzheimer’s patients might benefit from the shunting. The procedure is not something to take lightly. About 10 percent of people who had theshunt implanted experienced complications, while brain biopsies necessary to measure amyloid plaque and tangles is an invasive procedure.
A better and less invasive solution would be to look for biomarkers that would indicate too much cerebrospinal fluid using a spinal tap, a method Koga and his colleagues are currently investigating.
“When the disease is advanced and patients have this high number of lesions, they will not benefit from being shunted,” Koga said. “In the future, we could use biomarkers to predict which patients with dementia will benefit from shunting and which will not.”
Dr. Richard Byrne, chairman of neurosurgery at Rush University Medical Center, called the study an “intuitive, intelligent way” of trying to determine how to figure out which patients would be helped by shunt.
Currently, differentiating the two is difficult, Byrne added. Neurologists and neurosurgeons rely on a combination of the patient’s symptoms, physical exam, brain scans and draining fluid using a spinal tap to determine if patients show signs of improvement.
“Unfortunately, none of those are perfect tests,” Byrne said. “This is a very difficult web to untangle, and they are trying to add some more diagnostic tools. They seem to be making some strides in figuring it out.”
The other condition, normal pressure hydrocephalus (NPH), occurs when excess cerebrospinal fluid builds up in the ventricles, or cavities, deep within the brain. The reasons for the build-up of fluid are unknown, but it tends to occur in older people, said study author Dr. Sebastian Koga, a senior resident and surgeon in the department of neurosurgery at University of Virginia Health Science Center.
When diagnosing NPH, doctors look for three specific symptoms: difficulty walking (gait disturbances), urinary incontinence and dementia, or memory loss. The condition can often be slowed or relieved through a surgical procedure in which a shunt is implanted in the brain to drain fluid into the abdominal cavity, where it’s harmlessly reabsorbed, Koga said.
In the study, Koga and his colleagues took brain biopsies from 50 patients who had been diagnosed with NPH and who had shunt surgery.
About 30 percent had also been diagnosed with other conditions, including Parkinson’s-like tremors (13 percent), major depression (16 percent) and Alzheimer’s (3 percent).
After the surgery, the researchers followed patients for an average of 26 months. Nearly half (47 percent) had a significant improvement in their symptoms.
But about 21 percent saw no benefit and 30 percent continued to decline rapidly, Koga said.
In analyzing the brain tissue, the researchers found that the patients most likely to not improve or to decline also had high counts of amyloid plaques and neurofibrillary tangles, the hallmarks of Alzheimer’s disease.
While one possible conclusion is that these patients also had Alzheimer’s, another possibility is that both conditions share underlying similarities, and that shunting could also help some of those with Alzheimer’s, Koga said.
“Since 1965, we have been thinking this triage of symptoms — gait abnormality, urinary incontinence and memory problems — as a special disease and we have named it normal pressure hydrocephaly,” Koga said. “My hypothesis is that NPH is not a specific disease process, but part of a spectrum of dementia.”
The research was to be presented Tuesday at the American Association of Neurological Surgeons meeting in Philadelphia.
Since the 1960s, doctors have considered NPH a separate disease from Alzheimer’s, which occurs when beta-amyloid protein builds up and forms amyloid plaques and neurofibrillary tangles. The process is thought to kill neurons and lead to the degenerative symptoms of Alzheimer’s.
Instead of focusing on the symptoms of NPH, Koga argues, the two conditions may both be caused by tau-protein abnormalities. That means that some of those 5 million to 6 million people with Alzheimer’s may also benefit from shunting, something not typically offered to patients diagnosed with Alzheimer’s, he added.
“It’s theoretically possible that this same surgery could help forestall the symptoms or improve the symptoms of Alzheimer’s,” Koga said.
One challenge, however, is determining which Alzheimer’s patients might benefit from the shunting. The procedure is not something to take lightly. About 10 percent of people who had theshunt implanted experienced complications, while brain biopsies necessary to measure amyloid plaque and tangles is an invasive procedure.
A better and less invasive solution would be to look for biomarkers that would indicate too much cerebrospinal fluid using a spinal tap, a method Koga and his colleagues are currently investigating.
“When the disease is advanced and patients have this high number of lesions, they will not benefit from being shunted,” Koga said. “In the future, we could use biomarkers to predict which patients with dementia will benefit from shunting and which will not.”
Dr. Richard Byrne, chairman of neurosurgery at Rush University Medical Center, called the study an “intuitive, intelligent way” of trying to determine how to figure out which patients would be helped by shunt.
Currently, differentiating the two is difficult, Byrne added. Neurologists and neurosurgeons rely on a combination of the patient’s symptoms, physical exam, brain scans and draining fluid using a spinal tap to determine if patients show signs of improvement.
“Unfortunately, none of those are perfect tests,” Byrne said. “This is a very difficult web to untangle, and they are trying to add some more diagnostic tools. They seem to be making some strides in figuring it out.”
What we know about the meaning of dreams

What do we know about dreams - and their meaning? CNN writer Elizabeth Landau tackled that question in an article today and turned to well-known sleep researcher William Dement, MD:
Scientists know about as much about the dreaming brain as they do the waking brain -- in other words, there's still a lot to learn about how the brain creates the dreaming consciousness and wakeful consciousness, said William Dement, leading sleep researcher at Stanford University... You are conscious in your dreams in basically the same way you are conscious in real life, but you don't remember dreams as well because memory processing is down, Dement said. The continuity of real life experiences helps you distinguish waking life from the dream world. For example, you don't magically reappear in a different setting in the real world, whereas it might appear that way in a single night of dreaming.For more on the mystery of dreams, check out a Stanford Medicine piece I wrote a few years back.
"In some ways, it's very good we don't remember our dreams very well," he said. "You'd constantly be saying, 'Did that happen, or was it a dream?' "
The Dis-Ease of the Western Mind
When someone asked Gandhi what he thought of Western civilization, he replied that he thought it was a good idea. It is indeed a good idea, because it's not entirely a reality. Western civilization -- more exactly, the Western mind that creates the civilization -- has a serious disease. It's a "dis-ease" that affects all of us in the West. And now we can have a better idea of what's behind it.
Take merely these characteristics of the Western mind:
Are these traits purely accidental, just the way the typical Western mind happens to work?
A historical analysis can furnish an explanation why this particular mindset came to dominate the West. The main reason appears to be the separation of the world of values, feelings and spirit from the world of fact and reason at the dawn of the modern age. Following the famous trial of Giordano Bruno, the Church claimed for itself authority over the world of value, feeling and spirit, and allowed science and scientists to investigate the world of fact through reasoning based on observation and experiment.
The original covenant between science and church, concluded on the part of science by Galileo, was reinforced and made into an unquestioned precept by the radical separation of the two worlds by René Descartes. According to Cartesian philosophy there is a complete disjunction between the physical world "outside" the mind (the world of "extended substance" res extensa) and the thinking, feeling world "within" (the thinking substance, res cogitans). Science made great progress by dissecting the outside world into parts and manipulating the parts: this became the basis of modern technology. And the West fell in love with technology, more exactly, with the powers over people and nature conferred by technology. It relegated the felt "inside" world of value, feeling, and spirit to religion and spirituality, to be celebrated on Sundays and holidays. It made the manipulation of the "outside" world its true concern: the woof and wharf of modern economics and politics, the way relations between people, and between people and nature, are decided and conducted.
This historical backdrop might explain how it is that the West ended up with an impersonal, mechanical, atomized world as its "real" world. But it doesn't say how the Western mind actually operates, why it sees the world as an impersonal, mechanical aggregate of atomistic parts. But cognitive neuroscience can tell us more.
Roger Sperry, Michael Gazzaniga, and the other pioneers of split-brain research founded the discipline of cognitive neuroscience. They discovered that we have two brains and not just one. We have the right brain and the left brain -- more exactly, the right and the left hemisphere of the neocortex. The two brains are different in their functioning and even in their anatomy. The right hemisphere is wider, longer, larger and heavier than the left. It's also different in its sensitivity to neurotransmitters and neurohormones, and has a different neuronal structure and organization. It's differently "tuned" to our experience.
It's important to realize that the world is not given in experience in its pristine purity, "just the way it is." Input from our senses is organized, interpreted by our brain, with the result that the same sensory stimulus can give rise to very different experiences, very different interpretations. (Think of the famous drawing used by psychologists, where you can see either an elegant young woman, or an old hag.) Our two brains "see" the world each in its own way, and these ways are different. The reason that we have something like a single world-picture is because one of the two brains is dominant. In the West, the left brain is dominant. And here is the clue to the "dis-ease" of the Western mind.
In his seminal book The Master and His Emissary: The Divided Brain and the Making of the Western World, neuroscientist Iain McGilchrist asked, what would it look like if our left brain were the sole purveyor of reality? The whole world would be a heap of bits and pieces; its only meaning would come through its capacity to be used. Our attention would be narrowly focused on the individual bits and pieces, with increasing specialization bringing more and more familiarity with less and less. Information and information-gathering would be substituted for knowledge gained by actual experience. And the kind of knowledge we would gain would be rooted in representations of reality, by abstract cognitive schemes that would seem more "real" than the things we actually experience.
Does this world seem familiar? That shouldn't surprise you: the left-hemisphere's view of the world is by and large the Western mind's view of the world. There are people and things in this world, but there is no "betweenness" -- they are connected only by relations of cause and effect, by how one thing affects another, by what one person "does" to another. This world is centered on, and is best when it deals with, the things we ourselves have created. It's a competitive world, where everyone is separate, and everyone is out for him- or herself. And it's an impersonal and uncaring world, where to think that there is meaning, feeling, and purpose is merely to project one's own subjective feelings onto an impersonal "objective" reality.
The world of the right brain would be a very different world. Although having only the right brain available to us we would mean we couldn't analyze things and express them in language, our experience would be filled with many positive things. We would be making connections between things, seeing the world around us as a whole in which people and things are organic parts. We would be attending directly to our experience, seeing people and things in their presented uniqueness. We would be living in our body, feeling ourselves one with it and the world that surrounds and embeds it. The sense of time, the "flow" of things, would be primary, and we would enjoy experiences where this flow is evident, such as narration, theatre, dance, and music. Because of the betweenness connecting us to the world, we would be more empathetic, tuned to compassion and fellow-feeling, and concern with all things in nature. And our empathies would get a powerful boost by our being aware of our intuitions, of our subtle communication with the world beyond the range of our bodily senses. This perception is within the compass of the nonlocal quantum-receptivity of the sub-neuronal networks of our brain, but is repressed by the narrow rationality of our left hemisphere.
This right-brain world would seem more familiar to traditional people than to most of us in Western civilization. But to many of us it might seem more like regress than progress, for it would mean giving up much of our technical prowess and manipulative skills. However, this would not be necessary: we could also combine the world of our right brain with the world of the left. We could hand the things and events presented to our world-tuned right brain to the left for analysis, formulation, and communication, and then allow our right brain to place it in context, so we could reach an integral assessment and a balanced way of responding. We would see the forest, and still find our way among the trees.
The dis-ease of the Western mind is a product of historical circumstance. But it is not fated; we could overcome our one-sided heritage of the past. The key to it is using our brain more fully. This would give us a consciousness where the broad, holistic world of the right brain is linked with the pragmatic, skillful world of the left. This "broadband" consciousness without loss of acuity is the hallmark of what I called Quantum Consciousness. QC could be the next step in the evolution of the human mind, and it could be our salvation. Moving toward it by balancing your own approach to reality would be a good beginning toward curing the dis-ease of the Western mind.
Take merely these characteristics of the Western mind:
- it sees things as separate, each thing on its own, connected merely by mechanistic relations of cause and effect;
- it's competitive: each individual is on his or her own, making his or her way in an impersonal and indifferent world;
- it disconnects the mind from the body: the mind only "drives" or "manages" the body as it would a car or an organization;
- it best understands the things it creates as artificial, synthetic things that can be readily and unambiguously manipulated;
- it disconnects the human from the natural; nature itself becomes the "environment" that humans can manage and manipulate to serve their interests;
- it categorizes, schematizes people and things, viewing them as abstract entities rather than as existing, living realities;
- it deals with the representations of people and things rather than with our living experience of people and things;
- and it views all things, nature included, as mechanistic kinds of systems, put together from their parts and capable of being manipulated by acting on their parts.
Are these traits purely accidental, just the way the typical Western mind happens to work?
A historical analysis can furnish an explanation why this particular mindset came to dominate the West. The main reason appears to be the separation of the world of values, feelings and spirit from the world of fact and reason at the dawn of the modern age. Following the famous trial of Giordano Bruno, the Church claimed for itself authority over the world of value, feeling and spirit, and allowed science and scientists to investigate the world of fact through reasoning based on observation and experiment.
The original covenant between science and church, concluded on the part of science by Galileo, was reinforced and made into an unquestioned precept by the radical separation of the two worlds by René Descartes. According to Cartesian philosophy there is a complete disjunction between the physical world "outside" the mind (the world of "extended substance" res extensa) and the thinking, feeling world "within" (the thinking substance, res cogitans). Science made great progress by dissecting the outside world into parts and manipulating the parts: this became the basis of modern technology. And the West fell in love with technology, more exactly, with the powers over people and nature conferred by technology. It relegated the felt "inside" world of value, feeling, and spirit to religion and spirituality, to be celebrated on Sundays and holidays. It made the manipulation of the "outside" world its true concern: the woof and wharf of modern economics and politics, the way relations between people, and between people and nature, are decided and conducted.
This historical backdrop might explain how it is that the West ended up with an impersonal, mechanical, atomized world as its "real" world. But it doesn't say how the Western mind actually operates, why it sees the world as an impersonal, mechanical aggregate of atomistic parts. But cognitive neuroscience can tell us more.
Roger Sperry, Michael Gazzaniga, and the other pioneers of split-brain research founded the discipline of cognitive neuroscience. They discovered that we have two brains and not just one. We have the right brain and the left brain -- more exactly, the right and the left hemisphere of the neocortex. The two brains are different in their functioning and even in their anatomy. The right hemisphere is wider, longer, larger and heavier than the left. It's also different in its sensitivity to neurotransmitters and neurohormones, and has a different neuronal structure and organization. It's differently "tuned" to our experience.
It's important to realize that the world is not given in experience in its pristine purity, "just the way it is." Input from our senses is organized, interpreted by our brain, with the result that the same sensory stimulus can give rise to very different experiences, very different interpretations. (Think of the famous drawing used by psychologists, where you can see either an elegant young woman, or an old hag.) Our two brains "see" the world each in its own way, and these ways are different. The reason that we have something like a single world-picture is because one of the two brains is dominant. In the West, the left brain is dominant. And here is the clue to the "dis-ease" of the Western mind.
In his seminal book The Master and His Emissary: The Divided Brain and the Making of the Western World, neuroscientist Iain McGilchrist asked, what would it look like if our left brain were the sole purveyor of reality? The whole world would be a heap of bits and pieces; its only meaning would come through its capacity to be used. Our attention would be narrowly focused on the individual bits and pieces, with increasing specialization bringing more and more familiarity with less and less. Information and information-gathering would be substituted for knowledge gained by actual experience. And the kind of knowledge we would gain would be rooted in representations of reality, by abstract cognitive schemes that would seem more "real" than the things we actually experience.
Does this world seem familiar? That shouldn't surprise you: the left-hemisphere's view of the world is by and large the Western mind's view of the world. There are people and things in this world, but there is no "betweenness" -- they are connected only by relations of cause and effect, by how one thing affects another, by what one person "does" to another. This world is centered on, and is best when it deals with, the things we ourselves have created. It's a competitive world, where everyone is separate, and everyone is out for him- or herself. And it's an impersonal and uncaring world, where to think that there is meaning, feeling, and purpose is merely to project one's own subjective feelings onto an impersonal "objective" reality.
The world of the right brain would be a very different world. Although having only the right brain available to us we would mean we couldn't analyze things and express them in language, our experience would be filled with many positive things. We would be making connections between things, seeing the world around us as a whole in which people and things are organic parts. We would be attending directly to our experience, seeing people and things in their presented uniqueness. We would be living in our body, feeling ourselves one with it and the world that surrounds and embeds it. The sense of time, the "flow" of things, would be primary, and we would enjoy experiences where this flow is evident, such as narration, theatre, dance, and music. Because of the betweenness connecting us to the world, we would be more empathetic, tuned to compassion and fellow-feeling, and concern with all things in nature. And our empathies would get a powerful boost by our being aware of our intuitions, of our subtle communication with the world beyond the range of our bodily senses. This perception is within the compass of the nonlocal quantum-receptivity of the sub-neuronal networks of our brain, but is repressed by the narrow rationality of our left hemisphere.
This right-brain world would seem more familiar to traditional people than to most of us in Western civilization. But to many of us it might seem more like regress than progress, for it would mean giving up much of our technical prowess and manipulative skills. However, this would not be necessary: we could also combine the world of our right brain with the world of the left. We could hand the things and events presented to our world-tuned right brain to the left for analysis, formulation, and communication, and then allow our right brain to place it in context, so we could reach an integral assessment and a balanced way of responding. We would see the forest, and still find our way among the trees.
The dis-ease of the Western mind is a product of historical circumstance. But it is not fated; we could overcome our one-sided heritage of the past. The key to it is using our brain more fully. This would give us a consciousness where the broad, holistic world of the right brain is linked with the pragmatic, skillful world of the left. This "broadband" consciousness without loss of acuity is the hallmark of what I called Quantum Consciousness. QC could be the next step in the evolution of the human mind, and it could be our salvation. Moving toward it by balancing your own approach to reality would be a good beginning toward curing the dis-ease of the Western mind.
Former Acorn bod to simulate human brain

While IBM is looking to the processing might of its Blue Gene supercomputer to attempt to replicate the functions of the human brain, a former R&D whiz kid from Acorn is attempting to perform a similar feat using thousands of ARM-based processors.
The SpiNNaker project is headed up by Professor Stephen Furber, who worked at Acorn between 1980 and 1990, and was also a principal designer of both the BBC Micro and the 32-bit ARM RISC processor. Back then, the chip was designed for Acorn’s line of Archimedes computers, but the ARM architecture is now used widely in portable devices, from smartphones to the Nintendo DS.
The idea is that SpiNNaker will take advantage of mass-parallel processing to simulate the way in which neurons in the human brain communicate with each other, via electrical “spikes”. The system will comprise a huge array of ARM-based chips that are currently being fabricated in Taiwan, each of which will contain 20 ARM cores. In turn, each core will have access to its own block of SDRAM.
According to New Scientist, the SDRAM is needed to store the “changing synaptic weights as simple numbers that represent the importance of a given connection at any moment.”
According to Furber, these numbers will originally be loaded from the PC, but the machine will eventually be able to compute them itself as it becomes more intelligent. At that point, says Furber, “the only computer able to compute them will be the machine itself".
Each ARM core will have the job of modelling 1,000 virtual neurons, making for a total of 20,000 neurons per chip. The team hopes to be able to model a colossal total of a billion neurons with the highly parallel machine, meaning that the project will need 50,000 chips in total. This is still a way off in the future, but New Scientist reports that the team hopes to have a version with 10,000 processors up and running later this year.
Initially, Furber hopes to teach the self-learning brain to control a robotic arm, and then work towards controlling a humanoid robot. "Robots offer a natural, sensory environment for testing brain-like computers," he says. "You can instantly tell if it is being useful."
Furber isn’t the only person hoping to get close to virtually modelling a human brain. In 2008, IBM announced its own plans to build a system of virtual synapses and neurons using nanoscale devices. IBM also modelled a small mammal brain in 2008, but even this modest project required IBM’s colossal Blue Gene supercomputer project. Given the huge amount of computing power needed to emulate even basic brain, the chances of accurately modelling a whole human brain are remote.
However, Furber reckons that his low-cost approach offers a better doorway into modelling the human brain than IBM’s large-scale approach. "We're using bog-standard, off-the-shelf processors of fairly modest performance," he admits, pointing out that this is the best way to start modelling even a fraction of the flexibility of the human brain.
The SpiNNaker project is headed up by Professor Stephen Furber, who worked at Acorn between 1980 and 1990, and was also a principal designer of both the BBC Micro and the 32-bit ARM RISC processor. Back then, the chip was designed for Acorn’s line of Archimedes computers, but the ARM architecture is now used widely in portable devices, from smartphones to the Nintendo DS.
The idea is that SpiNNaker will take advantage of mass-parallel processing to simulate the way in which neurons in the human brain communicate with each other, via electrical “spikes”. The system will comprise a huge array of ARM-based chips that are currently being fabricated in Taiwan, each of which will contain 20 ARM cores. In turn, each core will have access to its own block of SDRAM.
According to New Scientist, the SDRAM is needed to store the “changing synaptic weights as simple numbers that represent the importance of a given connection at any moment.”
According to Furber, these numbers will originally be loaded from the PC, but the machine will eventually be able to compute them itself as it becomes more intelligent. At that point, says Furber, “the only computer able to compute them will be the machine itself".
Each ARM core will have the job of modelling 1,000 virtual neurons, making for a total of 20,000 neurons per chip. The team hopes to be able to model a colossal total of a billion neurons with the highly parallel machine, meaning that the project will need 50,000 chips in total. This is still a way off in the future, but New Scientist reports that the team hopes to have a version with 10,000 processors up and running later this year.
Initially, Furber hopes to teach the self-learning brain to control a robotic arm, and then work towards controlling a humanoid robot. "Robots offer a natural, sensory environment for testing brain-like computers," he says. "You can instantly tell if it is being useful."
Furber isn’t the only person hoping to get close to virtually modelling a human brain. In 2008, IBM announced its own plans to build a system of virtual synapses and neurons using nanoscale devices. IBM also modelled a small mammal brain in 2008, but even this modest project required IBM’s colossal Blue Gene supercomputer project. Given the huge amount of computing power needed to emulate even basic brain, the chances of accurately modelling a whole human brain are remote.
However, Furber reckons that his low-cost approach offers a better doorway into modelling the human brain than IBM’s large-scale approach. "We're using bog-standard, off-the-shelf processors of fairly modest performance," he admits, pointing out that this is the best way to start modelling even a fraction of the flexibility of the human brain.
Functional MRI in Brain Research

Our perceptions, thoughts, speech and decisions are carried out by a complex network of neurons that communicate through brief electrical impulses about one millisecond in duration (so called action potentials or ‘spikes’). These electrical impulses allows the brain to perform all its amazing computations in real time, such as recognizing faces, keeping your balance, and understanding speech. In other words, spikes are the currency of computation in the brain. To study how the brain is capable of these feats we need, therefore, to measure directly how populations of neurons communicate with each other by means of spiking activity.
A key challenge in this work is that neurons are very small (cell bodies are about 25 micrometer in diameter) and they are tightly packed together. As an analogy, consider a football stadium full of spectators. The problem is akin to developing a method to listen to the conversation between two individuals in the middle of this noisy crowd. Clearly, without getting a microphone close enough to them, the background noise would make the measurement nearly impossible. You cannot listen to an individual conversation with a microphone hanging in the middle of the stadium. The micro-electrode, an insulated wire with a diameter smaller than a human hair, is such a “microphone” that allows us to record the spikes of individual cells in the working brain by getting close enough to the individual cells.
Is there a way to measure the activity of single neurons non-invasively in humans? The answer is no. So what about functional MRI? fMRI does not measure neural activity directly, but instead relies on indirect changes in blood flow and volume triggered by modulation in neural activity. To begin with, it turns out that we we still do not know how fMRI measurements relate to neural activity. Clearly, to be able to understand how fMRI signals relate to neural activity we need to measure both simultaneously, work that will also require the use of animals. Importantly, fMRI has a limited spatial resolution of about a cubic millimeter. In such a volume, one can find in the order of 100,000 neurons. In other words, the ‘fMRI microphone’ cannot listen to individual cells, but to a whole stadium full of them. Finally, we already know that fMRI signals are much slower than neuronal activity, as the time course of hemodynamic signals is in the order of 5 seconds. As neurons work hundreds of of times faster (you can recognize an image in less than 150 ms), the dynamics of fMRI signals are too slow to understand how brains compute in real time. Instead, fMRI provides useful information about what brain areas might be involved in certain tasks. After these areas are identified, electrophysiological measurements with micro-electrodes can be used to measure the activity of single neurons in those areas. The combination of such tools is proving extremely useful in neuroscience research.
A couple of weeks ago animal right activists marched through UCLA carrying a sign saying “Support alternatives to animal research”. I was unsure whether to join them or not. After all, we fully support and work towards the development of alternative, non-invasive methods. Their sign, of course, is designed to suggest to the public that such methods currently exist and scientists refuse to use them. This is just not the case. Functional MRI is am extremely useful research useful tool, but not a replacement for electrophysiological work that requires measurement at micrometer scales.
In addition, Dr. Greek's claims that functional MRI and other imaging technologies were developed without the use of animals is simply untrue. In the case of functional MRI, it was the groundbreaking work of Owaga and colleagues at Bell Labs using rodents that showed that changes in the levels of deoxygenated haemoglobin in blood vessels changed the MR signal from water molecules surrounding them. Neural activity in the brain affects the the relative concentration of oxy- and deoxy-haemoglobin which then gives rise to an indirect measurement of neural activity through the the T2* weighted image intensity. They subsequently showed functional signals in human visual cortex based on the animal studies.
Through May 15: "The Brain from Planet X"

Have you seen Little Shop of Horrors? How about The Rocky Horror Show, or any of the grade-Z drive-in movies that inspired it? Then you've seen pretty much everything in Brain, which offers an invasion of gaylien Body Snatchers who would giggle at the word "snatcher." That's not necessarily bad, at least not bad for camp; after all, we know it's a spoof going in. Mystery Science Theater 3000 proved ingenious people can, in fact, find clever ways to spoof idiotic sci-fi movies; it's a shame the jokes in Brain are usually more chuckles than laugh lines. This is the kind of comedy your homophobic grandma might describe as risqué, and your mom might describe as cute. (I know, as I saw it with my mom and she called it cute.) It's not as much fun as Little Shop, nor are Bruce Kimmel's lyrics as witty as Howard Ashman's, but it's certainly catchy and manages real irony in "World of Tomorrow," this show's "Somewhere That's Green."
TAO's production of Brain boasts the same director, Josh Anderson (also its keyboardist), and much of the same cast and crew as last season's Reefer Madness. I preferred that show, but I've noticed real growth in several of TAO's regular performers in only a year. Heather Christopher in particular has found new ways to shade presentational characters; her nod toward Lucille Ball tips into Joan Crawford territory when X-traterrestrials zap her with a female empowerment gun. Russ Holm adds to his roster of continuously funny characters with a near-impersonation of Pat Buttram, and Amy Shephard is a double-espresso, dancing dynamo. Paul Purvine and Lauren O'Neill are right in their wheelhouses as sex-starved Space Invaders. Rob Taylor makes an effective Rod Serling stand-in.
The only questionable costuming is Taylor's had-to-be-intentional Pee Wee Herman getup. In a role written for a butch male, Louise Morgan spills charmingly out of her own costume as the assistant to one-star General Mills. Yeah, it's that kind of show. Is there a Colonel Sanders reference? You bet! Will the Brain's hypertrophic noggin resemble a coral reef, or two scoops of raspberry sherbet? Why not both?
As for singin' and steppin', it's too bad the performers weren't miked; they had a tough time competing with the band and (bonus points) a real theremin. A few soloists flailed at occasional keys in Thursday's preview, but the chorus articulated well throughout and braved a rousing dance ensemble, the "Brain Tap."
Taken for what it is, The Brain from Planet X is an entertaining trifle, but I encourage TAO to produce, cast and act farther outside its comfort zone. TAO bills itself as Oly's edgiest theatre company, but in 2010, a campy poke at late-1950s suburban mores feels safe as houses.
I’m Telling the Truth, Your Honor. Just Look at This Brain Scan!
.  As neuroscientists refine their techniques for imaging the brain, scans like the fMRI keep creeping toward the courtroom and getting closer to joining to polygraph tests as means to sort liars from truth-tellers through physiology. In Brooklyn, lawyer David Levin is now offering the fMRI brain scan of a witness as proof of her honesty. If the court accepts it, it could be the first time such a brain scan was ever admitted as evidence.
As neuroscientists refine their techniques for imaging the brain, scans like the fMRI keep creeping toward the courtroom and getting closer to joining to polygraph tests as means to sort liars from truth-tellers through physiology. In Brooklyn, lawyer David Levin is now offering the fMRI brain scan of a witness as proof of her honesty. If the court accepts it, it could be the first time such a brain scan was ever admitted as evidence.
For what would be a legal breakthrough, the case is a rather minor one: Levin’s client, Cynette Wilson, claims she was treated poorly at her job at a staffing center after filing a sexual harassment complaint. The lawyer found a coworker of Wilson’s to corroborate her story, but wanted to bolster his credibility. Wired.com reports:
It’s not yet clear whether the judge will allow the brain scan to be entered as evidence. If the judge does go for it, there could be big consequences; thanks to good ol’ legal precedent, allowing a brain scan into this small case would make it much easier to get them into larger cases. And with companies ready to peddle brain scans and lawyers always hungry for something to bolster their case, the floodgates could come crashing open.
Then again, maybe that’s not so bad, Ed Cheng of Brooklyn Law School told Wired.
 As neuroscientists refine their techniques for imaging the brain, scans like the fMRI keep creeping toward the courtroom and getting closer to joining to polygraph tests as means to sort liars from truth-tellers through physiology. In Brooklyn, lawyer David Levin is now offering the fMRI brain scan of a witness as proof of her honesty. If the court accepts it, it could be the first time such a brain scan was ever admitted as evidence.
As neuroscientists refine their techniques for imaging the brain, scans like the fMRI keep creeping toward the courtroom and getting closer to joining to polygraph tests as means to sort liars from truth-tellers through physiology. In Brooklyn, lawyer David Levin is now offering the fMRI brain scan of a witness as proof of her honesty. If the court accepts it, it could be the first time such a brain scan was ever admitted as evidence.For what would be a legal breakthrough, the case is a rather minor one: Levin’s client, Cynette Wilson, claims she was treated poorly at her job at a staffing center after filing a sexual harassment complaint. The lawyer found a coworker of Wilson’s to corroborate her story, but wanted to bolster his credibility. Wired.com reports:
So, Levin had the coworker undergo an fMRI brain scan by the company Cephos, which claims to provide “independent, scientific validation that someone is telling the truth.”
Laboratory studies using fMRI, which measures blood-oxygen levels in the brain, have suggested that when someone lies, the brain sends more blood to the ventrolateral area of the prefrontal cortex. In a very small number of studies, researchers have identified lying in study subjects (.pdf) with accuracy ranging from 76 percent to over 90 percent.
This seems crazy for several reasons. According to Wired.com’s account, the scan on the witness wasn’t completed until four years after he heard comments about Wilson. It’s debatable that fMRI images would be reliable enough to present as evidence in court even if a memory were fresh in your mind. But try remembering the exact wording of a conversation you heard in the spring of 2006.It’s not yet clear whether the judge will allow the brain scan to be entered as evidence. If the judge does go for it, there could be big consequences; thanks to good ol’ legal precedent, allowing a brain scan into this small case would make it much easier to get them into larger cases. And with companies ready to peddle brain scans and lawyers always hungry for something to bolster their case, the floodgates could come crashing open.
Then again, maybe that’s not so bad, Ed Cheng of Brooklyn Law School told Wired.
Humans, he pointed out, are terrible lie detectors and yet our legal system is based on allowing them to make those determinations. If slightly better than chance is the baseline, any improvement on that could be a reason to allow the evidence into court.
Researchers closer to explaining postpartum depression
Research from Toronto's Centre for Addiction and Mental Health has revealed that elevated levels of a brain protein called monoamine oxidase A could explain why postpartum blues are so common for new moms. The study used brain imaging to look at new mothers four to six days after delivery. Researchers found levels of monoamine oxidase A (MAO-A) were 43% greater during this time than in women who weren't pregnant. MAO-A levels were highest on the fifth day, usually when postpartum blues are most severe.
MAO-A removes chemicals in the brain such as serotonin, which helps a person maintain a normal mood. Greater MAO-A levels mean a person feels sad "Understanding the biology of postpartum blues is important because when it is severe it leads to clinical level postpartum depression," said researcher Dr. Jeffrey Meyer. The study was released Tuesday.
"We hope this information may be used in the future to create dietary supplements that could provide the nutrients removed by high MAO-A and lower the risk for postpartum depression," Meyer said.
MAO-A removes chemicals in the brain such as serotonin, which helps a person maintain a normal mood. Greater MAO-A levels mean a person feels sad "Understanding the biology of postpartum blues is important because when it is severe it leads to clinical level postpartum depression," said researcher Dr. Jeffrey Meyer. The study was released Tuesday.
"We hope this information may be used in the future to create dietary supplements that could provide the nutrients removed by high MAO-A and lower the risk for postpartum depression," Meyer said.
Narco Analysis and Brain mapping unconstitutional - SC
The Supreme Court today declared today that forced narco-analysis, brain-mapping tests and polygraph tests are violative of Article 20(3) of the Constitution of India. The apex court had reserved its order on a bunch of petitions challenging the investigative procedure more than two years ago on January 25, 2008.
Investigative techniques such as brain-mapping, narco-analysis and polygraph tests have been used in the investigation of a large number of high profile cases, including that of Abdul Karim Telgi, the Nithari killings and the Arushi murder case.
Petitions were moved before the Supreme Court between 2005 and 2007 by Santokoben Sharmanbhai Jadeja, accused of leading an underworld gang in Gujarat. K. Venkateswara Rao, a Tamil film producer, Dilip Kamath and independent Maharashtra Member of Legislative Assembly Anil Gote challenged the constitutional validity of these tests. The latter three are all prime accused in the stamp paper scam led by Telgi.
Today, a three-judge bench headed by incumbent Chief Justice K.G. Balakrishnan and Justices R.V. Raveendran and Dalveer Bhandari, today finally clarified the legal position on the issue. The Bench held, "We are of the considered opinion that no individual can be forced and subjected to such techniques involuntarily and by doing so it amounts to unwarranted intrusion of personal liberty." The court further went on to declare that the investigative techniques were an unconstitutional invasion of privacy enshrined in Article 21.
Recently, the Delhi High Court had restrained investigative agencies from conducting the tests on Maoist leader Kobad Ghandy, saying that their legality was pending in the apex court. Lawyer Rebecca M. John, counsel for Ghandy, told newswire IANS, “I am just overjoyed at the Supreme Court decision. I think this should have been done a long time back. Narco test is simply unconstitutional and the Supreme Court has upheld the rule of law.”
Noted civil liberties activist Prashant Bhushan welcoming the court’s decision told Bar & Bench, “It's absolutely correctly decided and a welcome judgement, thought quite delayed. It is a mental 3rd degree method of interrogation which causes severe trauma to the victims and is unreliable. The constitution prohibits compelling a person from answering question here you are completely drugging him and compelling to answer. It violates a person’s right to silence and privacy as you are basically opening up his brain.”
However the court has allowed the tests to be administered to persons with their consent while stressing National Human Rights Commission guidelines be strictly adhered to. The tests are highly favoured by the Union Government and its agencies who maintained through the hearings that these tests were crucial to the investigation of terror related offences and conspiracy to commit murder. The Centre had submitted that these tests gave clues to the investigating agencies and had no evidentiary value. The Centre stressed on the fact that “no invasive procedure” was used during the conduct of these tests and further argued that the law commission was of the opinion that such procedures were essentially for the conduct of effective investigation.
Senior Counsel Dushyant Dave was appointed as the Amicus Curiae to the Apex Court, while Solicitor General Ghoolam E. Vahanvati appeared for the Union of India. Senior Counsel C Sundaram appeared for the appellants who was briefed by Lawyers’ Knit & Co., Rajesh Mahale, Sanjay Hegde, Minakshi Grover, Bina Madhavan and Shuvojeet Roy.
This verdict comes as a major setback to investigating agencies across the country and a victory for civil liberties activists who have long argued against these practices.
Investigative techniques such as brain-mapping, narco-analysis and polygraph tests have been used in the investigation of a large number of high profile cases, including that of Abdul Karim Telgi, the Nithari killings and the Arushi murder case.
Petitions were moved before the Supreme Court between 2005 and 2007 by Santokoben Sharmanbhai Jadeja, accused of leading an underworld gang in Gujarat. K. Venkateswara Rao, a Tamil film producer, Dilip Kamath and independent Maharashtra Member of Legislative Assembly Anil Gote challenged the constitutional validity of these tests. The latter three are all prime accused in the stamp paper scam led by Telgi.
Today, a three-judge bench headed by incumbent Chief Justice K.G. Balakrishnan and Justices R.V. Raveendran and Dalveer Bhandari, today finally clarified the legal position on the issue. The Bench held, "We are of the considered opinion that no individual can be forced and subjected to such techniques involuntarily and by doing so it amounts to unwarranted intrusion of personal liberty." The court further went on to declare that the investigative techniques were an unconstitutional invasion of privacy enshrined in Article 21.
Recently, the Delhi High Court had restrained investigative agencies from conducting the tests on Maoist leader Kobad Ghandy, saying that their legality was pending in the apex court. Lawyer Rebecca M. John, counsel for Ghandy, told newswire IANS, “I am just overjoyed at the Supreme Court decision. I think this should have been done a long time back. Narco test is simply unconstitutional and the Supreme Court has upheld the rule of law.”
Noted civil liberties activist Prashant Bhushan welcoming the court’s decision told Bar & Bench, “It's absolutely correctly decided and a welcome judgement, thought quite delayed. It is a mental 3rd degree method of interrogation which causes severe trauma to the victims and is unreliable. The constitution prohibits compelling a person from answering question here you are completely drugging him and compelling to answer. It violates a person’s right to silence and privacy as you are basically opening up his brain.”
However the court has allowed the tests to be administered to persons with their consent while stressing National Human Rights Commission guidelines be strictly adhered to. The tests are highly favoured by the Union Government and its agencies who maintained through the hearings that these tests were crucial to the investigation of terror related offences and conspiracy to commit murder. The Centre had submitted that these tests gave clues to the investigating agencies and had no evidentiary value. The Centre stressed on the fact that “no invasive procedure” was used during the conduct of these tests and further argued that the law commission was of the opinion that such procedures were essentially for the conduct of effective investigation.
Senior Counsel Dushyant Dave was appointed as the Amicus Curiae to the Apex Court, while Solicitor General Ghoolam E. Vahanvati appeared for the Union of India. Senior Counsel C Sundaram appeared for the appellants who was briefed by Lawyers’ Knit & Co., Rajesh Mahale, Sanjay Hegde, Minakshi Grover, Bina Madhavan and Shuvojeet Roy.
This verdict comes as a major setback to investigating agencies across the country and a victory for civil liberties activists who have long argued against these practices.
Magnetic stimulation of the brain can ease drug-resistant depression, study shows
Daily application of magnetic stimulation to the brain for about 37 minutes can ease depression in patients who are not responding to antidepressants, researchers reported Monday. The procedure -- in effect, a mild form of electroconvulsive therapy, or ECT, which has been shown to be very effective against severe depression -- has been approved by the Food and Drug Administration since 2008, but critics have questioned its efficacy because of the lack of suitable blinded trials. That problem has arisen because of the difficulty of performing a sham procedure that recipients might think is an active procedure.
Dr. Mark George at the Medical University of South Carolina in Charleston and his colleagues got around this problem by developing an apparatus that mimics the effects of the magnetic stimulator without actually producing a magnetic field. The device causes a tapping on the skull similar to that produced by the real treatment and causes eyes to twitch in the same manner. Even the physicians who were treating patients were unable to tell if a device was real or simulated.
The researchers enrolled 190 patients who had suffered from depression for at least three months but less than five years and who had not responded to antidepressants. Half received the actual treatment every weekday for three weeks, while the rest received the sham treatment on the same schedule. Ninety percent of those in the sham group completed the study, compared with 86% of those in the treatment group.
The team reported in the Archives of General Psychiatry that 14.1% of those in the treatment group had their depression relieved, compared with 5.1% of those in the control group. When both groups were given the treatment for another three weeks, 30% responded.
"This study should help settle the debate about whether [the technique] works for depression," George said in a statement. Now the team can begin to investigate ways to improve its efficacy. One possible solution, as demonstrated in the study, is to extend the treatment period for longer durations.
The device uses a magnetic coil placed on the head that pulses about 3,000 times during each treatment, stimulating a minute electrical current in the brain. In the trial, the field was focused on the top left front part of the brain. The patient is conscious during the procedure and there appears to be no significant side effects. Patients can drive themselves home afterward.
In ECT, in contrast, electrodes placed against the skin emit an electrical current that passes through the brain, causing convulsions. Patients must be sedated and have to be driven home afterward. Clinical trials are testing the new technique against a variety of other problems, including tinnitus [ringing in the ears] and schizophrenia.
The study was funded by the National Institute of Mental Health.
Dr. Mark George at the Medical University of South Carolina in Charleston and his colleagues got around this problem by developing an apparatus that mimics the effects of the magnetic stimulator without actually producing a magnetic field. The device causes a tapping on the skull similar to that produced by the real treatment and causes eyes to twitch in the same manner. Even the physicians who were treating patients were unable to tell if a device was real or simulated.
The researchers enrolled 190 patients who had suffered from depression for at least three months but less than five years and who had not responded to antidepressants. Half received the actual treatment every weekday for three weeks, while the rest received the sham treatment on the same schedule. Ninety percent of those in the sham group completed the study, compared with 86% of those in the treatment group.
The team reported in the Archives of General Psychiatry that 14.1% of those in the treatment group had their depression relieved, compared with 5.1% of those in the control group. When both groups were given the treatment for another three weeks, 30% responded.
"This study should help settle the debate about whether [the technique] works for depression," George said in a statement. Now the team can begin to investigate ways to improve its efficacy. One possible solution, as demonstrated in the study, is to extend the treatment period for longer durations.
The device uses a magnetic coil placed on the head that pulses about 3,000 times during each treatment, stimulating a minute electrical current in the brain. In the trial, the field was focused on the top left front part of the brain. The patient is conscious during the procedure and there appears to be no significant side effects. Patients can drive themselves home afterward.
In ECT, in contrast, electrodes placed against the skin emit an electrical current that passes through the brain, causing convulsions. Patients must be sedated and have to be driven home afterward. Clinical trials are testing the new technique against a variety of other problems, including tinnitus [ringing in the ears] and schizophrenia.
The study was funded by the National Institute of Mental Health.
Depression 'treatable by electromagnetic therapy'
 WASHINGTON: Patients suffering from depression may find relief from treatments using electromagnetic stimulation, offering a possible alternative to mood-altering medications, a new study found.
WASHINGTON: Patients suffering from depression may find relief from treatments using electromagnetic stimulation, offering a possible alternative to mood-altering medications, a new study found.The research, which was released on Monday, tested 190 patients who had previously failed to respond to antidepressant drugs.
Patients were given at least three weeks of magnetic stimulation. Scientists found that the treatment led to remissions for 14 percent of them, and that most remained in remission for several months.
The treatment, known as repetitive transcranial magnetic stimulation (rTMS) offers future hope of a non-drug treatment for depression sufferers, although researchers said additional studies are needed.
"This study should help settle the debate about whether rTMS works for depression," said Mark George of the Medical University of South Carolina in Charleston, who led the research team.
"We can now follow up clues suggesting ways to improve its effectiveness, and hopefully further develop a potential new class of stimulation treatments for other brain disorders."
The treatment aims to jump-start the brain's mood-regulating circuitry by jolting the top left front section with an electromagnetic coil emitting 3,000 pulses over a 37-minute session.
Researchers said the treatments can be safely administered in a doctor's office with few side effects, unlike more invasive brain stimulation treatments, such as electroconvulsive therapy (ECT).
The US National Institute of Mental Health-funded research showed that although the treatment "has not yet lived up to early hopes that it might replace more invasive therapies, this study suggests that the treatment may be effective in at least some treatment-resistant patients," center director Thomas Insel said.
Exposure to smoke in the womb may lead to psychiatric problems, study shows
It's well known that smoking while pregnant isn't good for the baby, but new research shows it could also lead to psychological problems for that baby later in life.
Smoking during pregnancy can increase the need for medication in childhood and young adulthood, according to a study released Tuesday in Vancouver at the Pediatric Academic Societies annual meeting at the Vancouver Convention Centre.
Researchers found that adolescents who had been exposed to prenatal smoking were at increased risk for use of all psychiatric drugs, particularly those used to treat depression, attention-deficit/hyperactivity disorder (ADHD) and addiction, compared to non-exposed youths.
"Recent studies show that maternal smoking during pregnancy may interfere with brain development of the growing fetus," said Mikael Ekblad, 23, lead author of the study and a pediatric researcher at Turku University Hospital in Finland. "By avoiding smoking during pregnancy, all the later psychiatric problems caused by smoking exposure could be prevented."
Results of Ekblad's study show 12.3 per cent of the young adults studied had used psychiatric drugs. Of those, 19.2 per cent had been exposed to prenatal smoking.
"Smoking during pregnancy is still quite common, even though the knowledge of its harmful effects has risen in recent years," Ekblad said.
Young adults whose mothers smoked more than 10 cigarettes a day had the highest rate of psychiatric medication use at 16.9 per cent. The rate among youths whose mothers smoked fewer than 10 a day was 14.7 per cent, and among unexposed youths it was 11.7 per cent.
"There are animal studies that show that nicotine exposure interferes with brain development, in particular the differentiation of cells," Ekblad said, adding that prenatal exposure to smoke is only one reason for depression.
Ekblad said another study he co-authored made the link between smoking and smaller frontal lobes and cerebellums in newborns.
"These are the important regions for normal cognitive development, so we think that might be the mechanism," he said.
According to Physicians for a Smoke-Free Canada, in 2005, approximately one in eight women who gave birth in the past five years reported that they had smoked either daily or occasionally during their last pregnancy. Not all women quit smoking when they discover they are pregnant. A Health Canada report from 2001 found that 58 per cent of the women who smoked at the time of the survey reported that they had smoked during their most recent pregnancy.
Ekblad's study was done using information from the Finnish Medical Birth Register for all children born in Finland from 1987 to 1989. The researchers analyzed records on mothers' psychiatric in-patient care from 1969-1989 and children's use of psychiatric drugs.
The risk for medication use was similar in males and females, and the study was adjusted for risk factors such as maternal age, birth weight and the mother's previous in-patient care for mental disorders.
Exposure to prenatal smoking can also cause an increased risk for respiratory disease, ear infections and asthma when the baby reaches childhood, according to the Pediatric Academic Societies.
Smoking during pregnancy can increase the need for medication in childhood and young adulthood, according to a study released Tuesday in Vancouver at the Pediatric Academic Societies annual meeting at the Vancouver Convention Centre.
Researchers found that adolescents who had been exposed to prenatal smoking were at increased risk for use of all psychiatric drugs, particularly those used to treat depression, attention-deficit/hyperactivity disorder (ADHD) and addiction, compared to non-exposed youths.
"Recent studies show that maternal smoking during pregnancy may interfere with brain development of the growing fetus," said Mikael Ekblad, 23, lead author of the study and a pediatric researcher at Turku University Hospital in Finland. "By avoiding smoking during pregnancy, all the later psychiatric problems caused by smoking exposure could be prevented."
Results of Ekblad's study show 12.3 per cent of the young adults studied had used psychiatric drugs. Of those, 19.2 per cent had been exposed to prenatal smoking.
"Smoking during pregnancy is still quite common, even though the knowledge of its harmful effects has risen in recent years," Ekblad said.
Young adults whose mothers smoked more than 10 cigarettes a day had the highest rate of psychiatric medication use at 16.9 per cent. The rate among youths whose mothers smoked fewer than 10 a day was 14.7 per cent, and among unexposed youths it was 11.7 per cent.
"There are animal studies that show that nicotine exposure interferes with brain development, in particular the differentiation of cells," Ekblad said, adding that prenatal exposure to smoke is only one reason for depression.
Ekblad said another study he co-authored made the link between smoking and smaller frontal lobes and cerebellums in newborns.
"These are the important regions for normal cognitive development, so we think that might be the mechanism," he said.
According to Physicians for a Smoke-Free Canada, in 2005, approximately one in eight women who gave birth in the past five years reported that they had smoked either daily or occasionally during their last pregnancy. Not all women quit smoking when they discover they are pregnant. A Health Canada report from 2001 found that 58 per cent of the women who smoked at the time of the survey reported that they had smoked during their most recent pregnancy.
Ekblad's study was done using information from the Finnish Medical Birth Register for all children born in Finland from 1987 to 1989. The researchers analyzed records on mothers' psychiatric in-patient care from 1969-1989 and children's use of psychiatric drugs.
The risk for medication use was similar in males and females, and the study was adjusted for risk factors such as maternal age, birth weight and the mother's previous in-patient care for mental disorders.
Exposure to prenatal smoking can also cause an increased risk for respiratory disease, ear infections and asthma when the baby reaches childhood, according to the Pediatric Academic Societies.
Signs And Symptoms Of Seizures
Fοr thе brain tο work normally, іt needs аn organized, controlled аnԁ systematic release οf electrical impulses. Thеѕе allow thе brain tο ɡеt connected tο thе different body раrtѕ аnԁ аƖѕο hаνе command within itself.
Generally, a seizure οr аn ictus іѕ characterized bу аn abrupt shift οf behavior, usually brief, bесаυѕе οf a momentary alteration іn thе electrical activity οf thе brain. A сеrtаіn kind οf seizure саn ԁіѕрƖау several distinctive characteristics.
Depending οn thе type οf seizure, іt саn trουbƖе individuals іn various ways. Thеrе аrе several different feelings thаt affected individuals mау experience prior tο аn encounter аnԁ thеrе аrе symptoms throughout аnԁ аftеr a seizure.
AƖmοѕt a quarter οf thе people whο hаνе a seizure disorder experience peculiar sensations аƖѕο known аѕ auras before experiencing thе actual ictal stage.
If someone іѕ sensitive аnԁ attentive tο hіѕ auras, thеn іt mау аѕ well bе a warning thаt mау hеƖр іn preventing potential injuries οr harms.
Thе initial seizure symptoms οr warnings whісh involve thе main senses include feelings οf dj vu, unusual smell, sound οr taste, brief loss οf vision οr blurring, racing thουɡhtѕ, wеіrԁ stomach sensations οr a tingling feeling.
A person wіth аn impending seizure attack mау аƖѕο feel fеаr οr panic. Hе mау experience dizziness, headache, lightheadedness, nausea, οr numbness. Bυt take note thаt sometimes seizures ԁο nοt present аnу auras οr warnings.
Thе actual seizure phase mау take numerous distinctive forms. Few people whο аrе aware οf thеіr aura mау јυѕt hаνе a continuity οf thе warning. Fοr ѕοmе, іt mау develop іntο a partial seizure.
Those wіth seizure disorder mау experience thουɡht black out, confusion, deafness, аn electric shock sensation, loss οf consciousness, out οf body experience fοr a few аnԁ blurring οf vision during thе ictal phase.
Observable seizure signs mау include chewing actions, convulsion, speaking difficulty, drooling, fluttering eyelids, foot stomping, hand waving, inability tο mονе, incontinence, lip smacking, shaking οr trembling, ѕtаrіnɡ, stiffening, excessive sweating, teeth grinding, tongue biting, twitching movements аnԁ difficulty οf breathing.
Aftеr thе seizure іѕ a shift frοm thе ictal state tο thе normal state οf thе person. Thіѕ phase іѕ аƖѕο known аѕ thе post-ictal period. It indicates thе recuperation time οf thе brain. It mау continue frοm јυѕt a few minutes up tο several hours, depending οn a number οf aspects.
Thе condition οf a person аnԁ thе type οf seizure wіƖƖ determine thе length οf recovery period. If a person hаѕ a complex partial seizure, hіѕ level οf consciousness steadily gets better іn thе post-ictal phase јυѕt Ɩіkе a patient waking up frοm thе effects οf anesthesia. Thе signs аnԁ symptoms thаt come аbουt throughout thе post-ictal phase mау include memory loss аnԁ writing difficulty.
Thе person mау аƖѕο experience confusion, desolation аnԁ ԁіѕtrеѕѕ, fеаr, frustration аnԁ embarrassment. Physical indications аftеr a seizure mау possibly include bruising, speaking difficulty, different forms οf injury, fatigue thеn drowsiness, headache, nausea, thirst аnԁ mау hаνе thе urge tο urinate οr defecate.
Thе symptoms differ depending οn thе type οf seizure. Mοѕt οf thе time, a person wіth seizure disorder іѕ ƖіkеƖу tο hаνе аn identical type οf seizure еνеrу time thus thе symptoms wіƖƖ presumably bе similar.
Hοwеνеr, thіѕ ԁοеѕ nοt mean thаt anyone wіth seizure wіƖƖ come асrοѕѕ аƖƖ thе symptoms mentioned. AƖѕο, οthеr people mау hаνе a different experience whісh іѕ nοt included іn here.
Generally, a seizure οr аn ictus іѕ characterized bу аn abrupt shift οf behavior, usually brief, bесаυѕе οf a momentary alteration іn thе electrical activity οf thе brain. A сеrtаіn kind οf seizure саn ԁіѕрƖау several distinctive characteristics.
Depending οn thе type οf seizure, іt саn trουbƖе individuals іn various ways. Thеrе аrе several different feelings thаt affected individuals mау experience prior tο аn encounter аnԁ thеrе аrе symptoms throughout аnԁ аftеr a seizure.
AƖmοѕt a quarter οf thе people whο hаνе a seizure disorder experience peculiar sensations аƖѕο known аѕ auras before experiencing thе actual ictal stage.
If someone іѕ sensitive аnԁ attentive tο hіѕ auras, thеn іt mау аѕ well bе a warning thаt mау hеƖр іn preventing potential injuries οr harms.
Thе initial seizure symptoms οr warnings whісh involve thе main senses include feelings οf dj vu, unusual smell, sound οr taste, brief loss οf vision οr blurring, racing thουɡhtѕ, wеіrԁ stomach sensations οr a tingling feeling.
A person wіth аn impending seizure attack mау аƖѕο feel fеаr οr panic. Hе mау experience dizziness, headache, lightheadedness, nausea, οr numbness. Bυt take note thаt sometimes seizures ԁο nοt present аnу auras οr warnings.
Thе actual seizure phase mау take numerous distinctive forms. Few people whο аrе aware οf thеіr aura mау јυѕt hаνе a continuity οf thе warning. Fοr ѕοmе, іt mау develop іntο a partial seizure.
Those wіth seizure disorder mау experience thουɡht black out, confusion, deafness, аn electric shock sensation, loss οf consciousness, out οf body experience fοr a few аnԁ blurring οf vision during thе ictal phase.
Observable seizure signs mау include chewing actions, convulsion, speaking difficulty, drooling, fluttering eyelids, foot stomping, hand waving, inability tο mονе, incontinence, lip smacking, shaking οr trembling, ѕtаrіnɡ, stiffening, excessive sweating, teeth grinding, tongue biting, twitching movements аnԁ difficulty οf breathing.
Aftеr thе seizure іѕ a shift frοm thе ictal state tο thе normal state οf thе person. Thіѕ phase іѕ аƖѕο known аѕ thе post-ictal period. It indicates thе recuperation time οf thе brain. It mау continue frοm јυѕt a few minutes up tο several hours, depending οn a number οf aspects.
Thе condition οf a person аnԁ thе type οf seizure wіƖƖ determine thе length οf recovery period. If a person hаѕ a complex partial seizure, hіѕ level οf consciousness steadily gets better іn thе post-ictal phase јυѕt Ɩіkе a patient waking up frοm thе effects οf anesthesia. Thе signs аnԁ symptoms thаt come аbουt throughout thе post-ictal phase mау include memory loss аnԁ writing difficulty.
Thе person mау аƖѕο experience confusion, desolation аnԁ ԁіѕtrеѕѕ, fеаr, frustration аnԁ embarrassment. Physical indications аftеr a seizure mау possibly include bruising, speaking difficulty, different forms οf injury, fatigue thеn drowsiness, headache, nausea, thirst аnԁ mау hаνе thе urge tο urinate οr defecate.
Thе symptoms differ depending οn thе type οf seizure. Mοѕt οf thе time, a person wіth seizure disorder іѕ ƖіkеƖу tο hаνе аn identical type οf seizure еνеrу time thus thе symptoms wіƖƖ presumably bе similar.
Hοwеνеr, thіѕ ԁοеѕ nοt mean thаt anyone wіth seizure wіƖƖ come асrοѕѕ аƖƖ thе symptoms mentioned. AƖѕο, οthеr people mау hаνе a different experience whісh іѕ nοt included іn here.
SC rules against forced narco anlaysis, lie detector tests
The Supreme Court has ruled that forcing someone to go through brain-mapping, narco-analysis or lie detector tests is unconstitutional because "it is an unwarranted intrusion on the individual's rights." (Read: What is narco analysis)
The verdict is a serious setback for the Central Bureau of Investigation ( CBI ) which argued that all their tests are legally sanctioned and are critical in cases where they can help provide evidence of crimes being committed.
The court, however, held that Article 20 (3) of the India Constitution that states "no person accused of any offence shall be compelled to be a witness against himself."
If a person volunteers to go through narco-analysis or brain-mapping, the findings cannot be used without other supporting evidence, said the court. Also, while conducting these tests, investigating agencies have to follow the guidelines of the National Human Rights Commission (NHRC).
The case against these forms of interrogation and investigation was moved, among others, by Santokben Sharmanbhai Jadeja, a woman accused of leading an underworld gang in Gujarat, and Tamil film producer K Venkateswara Rao.
The Delhi High Court had also recently restrained police from going ahead with narco-analysis for arrested Naxal leader Kobad Ghandy till the Supreme Court gave its ruling. (With PTI inputs)
The verdict is a serious setback for the Central Bureau of Investigation ( CBI ) which argued that all their tests are legally sanctioned and are critical in cases where they can help provide evidence of crimes being committed.
The court, however, held that Article 20 (3) of the India Constitution that states "no person accused of any offence shall be compelled to be a witness against himself."
If a person volunteers to go through narco-analysis or brain-mapping, the findings cannot be used without other supporting evidence, said the court. Also, while conducting these tests, investigating agencies have to follow the guidelines of the National Human Rights Commission (NHRC).
The case against these forms of interrogation and investigation was moved, among others, by Santokben Sharmanbhai Jadeja, a woman accused of leading an underworld gang in Gujarat, and Tamil film producer K Venkateswara Rao.
The Delhi High Court had also recently restrained police from going ahead with narco-analysis for arrested Naxal leader Kobad Ghandy till the Supreme Court gave its ruling. (With PTI inputs)
Big payout for Bristol teenager who suffered brain injury at birth
A judge yesterday told the family of 18-year-old Marcus Glassenbury he hoped they would now be able to "breathe a sigh of relief and move on" after a deal was reached to compensate him for his "pain and suffering" and to cover the enormous costs of the care he will need for the rest of his life.
A High Court hearing in London was told that Marcus, of Davis Street, Avonmouth, suffers from "severe developmental problems" due to cerebral palsy said to have been caused by two devastating brain haemorrhages in the hours after his birth in March 1992.
He cannot walk unaided, has limited communication abilities and needs round- the-clock care.
Marcus was born at Southmead Hospital after medics diagnosed a "placental abruption" in his mother Deborah Glassenbury, a serious complication in a pregnancy in which the lining of the placenta ruptures and separates from the womb.
The condition is the most common cause of bleeding in late pregnancy, affecting one in every 100 to 200 pregnancies, and can threaten the life of the baby and mother.
Surgeons carried out an emergency caesarean delivery at 29 weeks, but the rupture allegedly resulted in Marcus's post-birth brain haemorrhages.
Marcus – through his grandmother Angela Russell, of Pill – claimed damages from his mother's then GP, Dr Fiona Short, alleging negligence in failing to arrange a speedier hospital referral.
Dr Short – who was then practising from the Shirehampton Health Centre, in Pembroke Road, Shirehampton – denies negligence and liability. She is no longer listed as a doctor based at the practice.
Marcus's QC, Robin Oppenheim, yesterday told High Court judge Mr Justice Foskett a "compromise settlement" had been reached between the two parties.
It means Marcus will receive "substantial" compensation for his "pain and suffering" and to cover the enormous costs of the care he will need for the rest of his life.
Although the terms of the settlement have been kept confidential, millions of pounds are frequently awarded by the courts in similar cases.
Marcus's case had been prepared by Magi Young, a clinical negligence solicitor who specialises in cases of maximum severity.
Ms Young, a partner in specialist firm Parlett Kent, recently gained an award of £1.8 million for an undiagnosed brain injury.
On another case, an award of £1.2 million for blindness was made after an undiagnosed pituitary tumour.
Mr Oppenheim said Dr Short had visited and examined Marcus's mother early on the day of his birth, when Mrs Glassenbury complained of intense stomach pain.
Dr Short diagnosed a "urinary tract infection", a diagnosis which Mr Oppenheim argued "shouldn't have been made", although emphasising that "liability in respect of that consultation is still very much in dispute".
When Mrs Glassenbury reached hospital that night she was in a "state of shock", he said, and staff rushed her in for emergency surgery after identifying the placental rupture.
Mr Oppenheim claimed earlier diagnosis would have resulted in prompt resolution of the problem, with Mrs Glassenbury's baby proceeding to "full term".
Dr Short's QC, Edward Faulks, stressed that the settlement had been reached without admission of liability but said that the GP was "extremely pleased" that "a large sum of money should be paid to the family for the benefit of Marcus".
Mr Oppenheim said that Mrs Glassenbury and her family had provided Marcus with "unstinting care over the past 18 years".
Mr Justice Foskett, who approved the settlement, told relatives: "It has not been easy, but I hope this makes things easier for you".
Addressing Marcus's grandmother as she sat in court, he added: "This is a significant sum which should make a difference to his life."
He said the family could now "breathe a sigh of relief and move on".
Marcus's parents and grandmother declined to comment on the settlement when contacted by the Evening Post yesterday.
A High Court hearing in London was told that Marcus, of Davis Street, Avonmouth, suffers from "severe developmental problems" due to cerebral palsy said to have been caused by two devastating brain haemorrhages in the hours after his birth in March 1992.
He cannot walk unaided, has limited communication abilities and needs round- the-clock care.
The condition is the most common cause of bleeding in late pregnancy, affecting one in every 100 to 200 pregnancies, and can threaten the life of the baby and mother.
Surgeons carried out an emergency caesarean delivery at 29 weeks, but the rupture allegedly resulted in Marcus's post-birth brain haemorrhages.
Marcus – through his grandmother Angela Russell, of Pill – claimed damages from his mother's then GP, Dr Fiona Short, alleging negligence in failing to arrange a speedier hospital referral.
Dr Short – who was then practising from the Shirehampton Health Centre, in Pembroke Road, Shirehampton – denies negligence and liability. She is no longer listed as a doctor based at the practice.
Marcus's QC, Robin Oppenheim, yesterday told High Court judge Mr Justice Foskett a "compromise settlement" had been reached between the two parties.
It means Marcus will receive "substantial" compensation for his "pain and suffering" and to cover the enormous costs of the care he will need for the rest of his life.
Although the terms of the settlement have been kept confidential, millions of pounds are frequently awarded by the courts in similar cases.
Marcus's case had been prepared by Magi Young, a clinical negligence solicitor who specialises in cases of maximum severity.
Ms Young, a partner in specialist firm Parlett Kent, recently gained an award of £1.8 million for an undiagnosed brain injury.
On another case, an award of £1.2 million for blindness was made after an undiagnosed pituitary tumour.
Mr Oppenheim said Dr Short had visited and examined Marcus's mother early on the day of his birth, when Mrs Glassenbury complained of intense stomach pain.
Dr Short diagnosed a "urinary tract infection", a diagnosis which Mr Oppenheim argued "shouldn't have been made", although emphasising that "liability in respect of that consultation is still very much in dispute".
When Mrs Glassenbury reached hospital that night she was in a "state of shock", he said, and staff rushed her in for emergency surgery after identifying the placental rupture.
Mr Oppenheim claimed earlier diagnosis would have resulted in prompt resolution of the problem, with Mrs Glassenbury's baby proceeding to "full term".
Dr Short's QC, Edward Faulks, stressed that the settlement had been reached without admission of liability but said that the GP was "extremely pleased" that "a large sum of money should be paid to the family for the benefit of Marcus".
Mr Oppenheim said that Mrs Glassenbury and her family had provided Marcus with "unstinting care over the past 18 years".
Mr Justice Foskett, who approved the settlement, told relatives: "It has not been easy, but I hope this makes things easier for you".
Addressing Marcus's grandmother as she sat in court, he added: "This is a significant sum which should make a difference to his life."
He said the family could now "breathe a sigh of relief and move on".
Marcus's parents and grandmother declined to comment on the settlement when contacted by the Evening Post yesterday.
How I beat a rare brain bug but then had to learn to walk and talk again
Heather West battled for her life and spent six months in hospital after a bout of flu led to an illness so rare it affects only eight in a million people each year.
A year ago, she was confined to a hospital bed and only able to communicate by wiggling her finger.
The 27-year-old has made an amazing recovery and has signed up for Sunday's Race For Life, in aid of Cancer Research UK.
Heather, of Ettrick Drive, Sinfin, said: "Walking the circuit will be an achievement and I hope it will inspire people."
Her dad, Malcolm, said: "I'm very proud. This time last year Heather had to be hoisted out of bed and could barely feed herself."
Mum Julia described it as "like trying to wake up from a nightmare".
Waiting in hospital for the results of their daughter's brain scan, Malcolm and Julia looked on helplessly as Heather lost the ability to walk and talk within the space of just a few hours.
She had woken in the morning able to move about and communicate, but by lunchtime could not even swallow.
One of the last things she said was to tell her work she would not be in that day.
By the time the test results came through she was oblivious to the world around her.
Medics told Malcolm and Julia their daughter had damage to three areas of her brain which they would attempt to treat with heavy doses of drugs.
But they warned that she could die.
Julia, 50, of Ettrick Drive, Sinfin, said: "We couldn't believe the speed at which she got that poorly.
"She stopped talking in the morning and by lunchtime she couldn't walk or swallow.
"We were absolutely gobsmacked when they told us what was wrong. I kept describing it to people as like trying to wake up from a nightmare."
Heather had the rare brain disease acute disseminated encephalomyelitis – which is usually triggered by a viral infection and affects just eight in a million people per year.
Her diagnosis in February last year was the start of a six-month battle towards recovery.
During that time, she went from being unable to breathe by herself to getting out of her wheelchair and walking through the door of her home.
It all began with a bout of flu in December 2008.
Heather had been in good health throughout her life and appeared to have recovered from the flu, but in February she started suffering with migraines and double vision and was unsteady on her feet.
She went to her GP, who suspected it could be vertigo and gave her medication.
But when her condition failed to improve after about 10 days, Malcolm took her to casualty at the former Derbyshire Royal Infirmary.
Malcolm, 49, a laboratory manager at Burton's Queen's Hospital, said: "Because she's always been healthy she clearly wasn't right.
"I work in the NHS and alarm bells were ringing."
Heather was given a scan which did not detect any problems, so she was sent home with a follow-up appointment.
But the next day her speech slowed and she had slight difficulties walking.
The following morning, Malcolm and Julia thought she had suffered a stroke because the left side of her face had dropped.
They rushed her back to hospital and she was admitted immediately.
Because it was a Sunday, she had to wait until the following day to have a brain scan, which is when she was diagnosed.
She was transferred to Nottingham's Queen's Medical Centre, where she spent a week on a medical ward before her condition got even worse and she went into intensive care.
Julia and Malcolm took time off work and their son, David, travelled from his home in Surrey to be with them.
Malcolm said: "We started taking each day as it came. That was all we could do."
The family fell into a pattern of living off ready meals and spending visiting hours at the hospital, where they would sit and read to Heather in the hope she could still hear.
Malcolm completed all seven books of the Chronicles of Narnia and got halfway through the Harry Potter series.
Julia, who works in intensive care at Royal Derby Hospital, said: "Maybe our medical backgrounds helped us cope.
"I'd only been working in intensive care for a year and I kept saying what a time to have taken on that job. It helped because we weren't as fazed about everything."
Four weeks into Heather's hospital stay, she was given a second brain scan which showed that the damage had got worse.
Malcolm and Julia had not been prepared for this news, as they had believed Heather was improving because she had started moving a finger.
Despite the bad news of the scan, soon afterwards the improvements were definite and marked.
Heather started to breathe a bit on her own and her eyes, which had been looking in different directions, started to get better.
Malcolm said: "It had been horrible because one eye was looking one way and the other another, so it was as though no-one was looking back at me.
"When she started to improve we would see new things every day.
"Just seeing her toes wiggle was one of the biggest moments, because I knew that if they were moving then there was a good chance that the rest of her body, between her feet and her brain, had a good chance of getting better."
Heather left intensive care after six weeks and then spent the next three months on a ward for brain patients at Queen's Medical Centre.
Her rapid improvement continued, such as communicating by raising her finger for "yes" and curling it down for "no".
Malcolm and Julia do not remember some of the big moments in their daughter's recovery, such as the first time she spoke.
Malcolm said: "There weren't so many 'eureka' moments. It was more gradual.
"But it was quick enough that it felt like watching a child grow up at high speed.
"She went through the naughty phases that children go through – I'd tell her to suck a lolly and she'd bite it straightaway.
"She ripped her feeding tube out three times."
The first thing Heather remembers is her birthday, April 16, nearly two months after she was admitted to hospital.
She said: "I remember presents and cards and people visiting. And I had fruit juice on a sponge because I wasn't swallowing."
As she got better, she began having speech therapy to retrain her damaged brain to control the muscles in her mouth and tongue.
Heather said: "I remember the speech therapist asking if I could say 'banana' because 'b' was a difficult letter and I said 'nanas and custard'."
She was determined to get well as quickly as possible and, after four months in hospital, was weaned off much of her medication and moved to Royal Derby Hospital for intensive rehabilitation.
Malcolm said: "She was always determined and that was what helped her through.
"I can't imagine what it must have been like for her to come round in a hospital bed and find nothing in her body was working."
Heather was told that once she could walk again she could leave hospital.
She was so determined that she managed to do so in almost half the 12 weeks predicted, and was finally discharged on August 26 last year, six months after she was first taken into hospital.
Malcolm said: "We put ramps in place for her at home so we could bring her inside in a wheelchair.
"But she came home and walked straight through the door."
She still had a lot of recovering to do once she got home but her family agree that being without the care of hospital staff forced her to become more independent.
She has improved so much she is now able to lead a fairly regular life.
She still gets very tired but is able to drive again and, two months ago, returned to work as a credit controller in Burton.
Malcolm said: "It's changed our outlook on life in terms of what's important.
"We were burgled last week and they took a few things like a digital camera, but it's only stuff, it doesn't matter."
Julia said the experience had made her a better nurse.
She said: "I've always been very aware of patients' families and, although I've always tried to empathise, I believe I really can now.
"But when I see young people in intensive care I think back a bit. It's a bit of a flashback."
The family has thanked everyone who helped care for their daughter and they are now looking forward to their future together.
Malcolm said: "It's about making the most of the time you're here."
A year ago, she was confined to a hospital bed and only able to communicate by wiggling her finger.
The 27-year-old has made an amazing recovery and has signed up for Sunday's Race For Life, in aid of Cancer Research UK.
Heather, of Ettrick Drive, Sinfin, said: "Walking the circuit will be an achievement and I hope it will inspire people."
Her dad, Malcolm, said: "I'm very proud. This time last year Heather had to be hoisted out of bed and could barely feed herself."
Mum Julia described it as "like trying to wake up from a nightmare".
Waiting in hospital for the results of their daughter's brain scan, Malcolm and Julia looked on helplessly as Heather lost the ability to walk and talk within the space of just a few hours.
She had woken in the morning able to move about and communicate, but by lunchtime could not even swallow.
One of the last things she said was to tell her work she would not be in that day.
By the time the test results came through she was oblivious to the world around her.
Medics told Malcolm and Julia their daughter had damage to three areas of her brain which they would attempt to treat with heavy doses of drugs.
But they warned that she could die.
Julia, 50, of Ettrick Drive, Sinfin, said: "We couldn't believe the speed at which she got that poorly.
"She stopped talking in the morning and by lunchtime she couldn't walk or swallow.
"We were absolutely gobsmacked when they told us what was wrong. I kept describing it to people as like trying to wake up from a nightmare."
Heather had the rare brain disease acute disseminated encephalomyelitis – which is usually triggered by a viral infection and affects just eight in a million people per year.
Her diagnosis in February last year was the start of a six-month battle towards recovery.
During that time, she went from being unable to breathe by herself to getting out of her wheelchair and walking through the door of her home.
It all began with a bout of flu in December 2008.
Heather had been in good health throughout her life and appeared to have recovered from the flu, but in February she started suffering with migraines and double vision and was unsteady on her feet.
She went to her GP, who suspected it could be vertigo and gave her medication.
But when her condition failed to improve after about 10 days, Malcolm took her to casualty at the former Derbyshire Royal Infirmary.
Malcolm, 49, a laboratory manager at Burton's Queen's Hospital, said: "Because she's always been healthy she clearly wasn't right.
"I work in the NHS and alarm bells were ringing."
Heather was given a scan which did not detect any problems, so she was sent home with a follow-up appointment.
But the next day her speech slowed and she had slight difficulties walking.
The following morning, Malcolm and Julia thought she had suffered a stroke because the left side of her face had dropped.
They rushed her back to hospital and she was admitted immediately.
Because it was a Sunday, she had to wait until the following day to have a brain scan, which is when she was diagnosed.
She was transferred to Nottingham's Queen's Medical Centre, where she spent a week on a medical ward before her condition got even worse and she went into intensive care.
Julia and Malcolm took time off work and their son, David, travelled from his home in Surrey to be with them.
Malcolm said: "We started taking each day as it came. That was all we could do."
The family fell into a pattern of living off ready meals and spending visiting hours at the hospital, where they would sit and read to Heather in the hope she could still hear.
Malcolm completed all seven books of the Chronicles of Narnia and got halfway through the Harry Potter series.
Julia, who works in intensive care at Royal Derby Hospital, said: "Maybe our medical backgrounds helped us cope.
"I'd only been working in intensive care for a year and I kept saying what a time to have taken on that job. It helped because we weren't as fazed about everything."
Four weeks into Heather's hospital stay, she was given a second brain scan which showed that the damage had got worse.
Malcolm and Julia had not been prepared for this news, as they had believed Heather was improving because she had started moving a finger.
Despite the bad news of the scan, soon afterwards the improvements were definite and marked.
Heather started to breathe a bit on her own and her eyes, which had been looking in different directions, started to get better.
Malcolm said: "It had been horrible because one eye was looking one way and the other another, so it was as though no-one was looking back at me.
"When she started to improve we would see new things every day.
"Just seeing her toes wiggle was one of the biggest moments, because I knew that if they were moving then there was a good chance that the rest of her body, between her feet and her brain, had a good chance of getting better."
Heather left intensive care after six weeks and then spent the next three months on a ward for brain patients at Queen's Medical Centre.
Her rapid improvement continued, such as communicating by raising her finger for "yes" and curling it down for "no".
Malcolm and Julia do not remember some of the big moments in their daughter's recovery, such as the first time she spoke.
Malcolm said: "There weren't so many 'eureka' moments. It was more gradual.
"But it was quick enough that it felt like watching a child grow up at high speed.
"She went through the naughty phases that children go through – I'd tell her to suck a lolly and she'd bite it straightaway.
"She ripped her feeding tube out three times."
The first thing Heather remembers is her birthday, April 16, nearly two months after she was admitted to hospital.
She said: "I remember presents and cards and people visiting. And I had fruit juice on a sponge because I wasn't swallowing."
As she got better, she began having speech therapy to retrain her damaged brain to control the muscles in her mouth and tongue.
Heather said: "I remember the speech therapist asking if I could say 'banana' because 'b' was a difficult letter and I said 'nanas and custard'."
She was determined to get well as quickly as possible and, after four months in hospital, was weaned off much of her medication and moved to Royal Derby Hospital for intensive rehabilitation.
Malcolm said: "She was always determined and that was what helped her through.
"I can't imagine what it must have been like for her to come round in a hospital bed and find nothing in her body was working."
Heather was told that once she could walk again she could leave hospital.
She was so determined that she managed to do so in almost half the 12 weeks predicted, and was finally discharged on August 26 last year, six months after she was first taken into hospital.
Malcolm said: "We put ramps in place for her at home so we could bring her inside in a wheelchair.
"But she came home and walked straight through the door."
She still had a lot of recovering to do once she got home but her family agree that being without the care of hospital staff forced her to become more independent.
She has improved so much she is now able to lead a fairly regular life.
She still gets very tired but is able to drive again and, two months ago, returned to work as a credit controller in Burton.
Malcolm said: "It's changed our outlook on life in terms of what's important.
"We were burgled last week and they took a few things like a digital camera, but it's only stuff, it doesn't matter."
Julia said the experience had made her a better nurse.
She said: "I've always been very aware of patients' families and, although I've always tried to empathise, I believe I really can now.
"But when I see young people in intensive care I think back a bit. It's a bit of a flashback."
The family has thanked everyone who helped care for their daughter and they are now looking forward to their future together.
Malcolm said: "It's about making the most of the time you're here."
Subscribe to:
Comments (Atom)